http://news.yahoo.com/s/ap/20091027/ap_on_bi_ge/us_health_care_overhaul
By DAVID ESPO, AP Special Correspondent David Espo, Ap Special Correspondent – 1 hr 3 mins ago
WASHINGTON – Democratic moderates who control the balance of power on health care legislation balked Tuesday at a government-run insurance option for millions of Americans, underscoring the enormity of the challenge confronting Senate Majority Leader Harry Reid one day after he unveiled the plan as a consensus product.
Republican opposition stiffened, and party leaders announced they would attempt to strangle the bill before formal debate begins.
Despite the obvious obstacles, senior Democrats cast Reid's draft legislation as a turning point in the yearlong campaign to enact President Barack Obama's top domestic priority. Sen. Max Baucus, D-Mont., chairman of the Senate Finance Committee, said there is now a "sense of inevitability, the sense that, yes, we're going to pass health care reform, and it's going to lower costs, provide better health insurance coverage ... and reform the health insurance market."
The proposed government insurance option long ago emerged as the biggest flashpoint in both the House and Senate as Democrats struggle to pass legislation that extends coverage to millions who lack it, bans insurance industry practices such as denying coverage on the basis of pre-existing medical conditions and slows the growth of health care spending nationally.
But before that issue can be joined on the Senate floor, Reid's first challenge is to gain 60 votes — the number needed to overcome a filibuster by Republicans — just to bring the bill up, a parliamentary maneuver so routine that a vote is rarely required.
Sen. Mitch McConnell of Kentucky, the Republican leader, announced that in this case, members of his party will treat it as though it were "a vote on the merits" of a bill he said would "cut Medicare, raise taxes and increase health insurance premiums." He suggested Democrats could expect campaign commercials next year on the basis of the vote, and recalled that Sen. John Kerry, D-Mass., was ridiculed in his 2004 presidential campaign for having once said he voted for a bill before he voted against it.
Tuesday's developments illustrated the difficulties facing the 69-year-old Reid, juggling at least three separate concerns: his role as head of the Democratic caucus, the desire to deliver on Obama's agenda and a 2010 re-election campaign in Nevada, where his approval ratings are low.
"This isn't over until I'm standing with President Obama and he's signing a bill into law that delivers what Nevadans are demanding — real health insurance reform," Reid wrote in an e-mail message to political supporters in his home state Monday night.
The decision to include a government insurance option in his legislation had obvious appeal for liberals who account for a strong majority inside the Senate Democratic caucus, and it is likely to please labor unions and party activists in Nevada.
But it has gained less-than-effusive support from Obama, who is eager to have at least a dollop of bipartisanship for his signature domestic issue. Sen. Olympia Snowe of Maine, the only Republican who has sided with Democrats in committee this year, has announced she will not support the bill Reid drafted.
Still, if Reid is pressed in coming weeks by moderates to fall back, he can explain to liberals that he was forced to do so because his preference — a government insurance option — proved to be unobtainable in the Senate.
Already, that pressure is evident.
Sen. Tom Carper, D-Del., one of several Democrats unhappy with Reid's proposal, said he may seek changes on the Senate floor, a move likely to be welcomed by moderates. He backs a government role in states where one or two insurers control the market and premiums are high.
While Reid is expected eventually to secure all 60 Democratic votes on the critical first test to bring the bill to the Senate floor, Sens. Ben Nelson of Nebraska, Mary Landrieu of Louisiana and Evan Bayh of Indiana all declined to say on Tuesday how they would vote.
In an indication of the pressure Reid faces, Bayh said the majority leader had agreed to cut an earlier proposal for a $40 billion tax on medical device makers.
"He significantly modified that proposal in a way that I understand will not impact thousands of good-paying jobs," said Bayh, whose state is home to Guidant Corp., a maker of cardiovascular devices, among other major industry players. No details were available on the precise changes Reid agreed to.
Speaker Nancy Pelosi is in a similar position in the House. Efforts to draft a consensus health care bill for a vote have been stalled for more than two weeks. The principal stumbling block is an internal disagreement over terms for setting fees for doctors, hospitals and other health care providers treating patients with government-sold coverage.
Liberals want the government to set the rate unilaterally, pegged to the charges the government pays Medicare beneficiaries. Moderates want the government to negotiate with the providers in setting fees.
Pelosi favors the approach liberals want, but officials say she has all but concluded she cannot gain the necessary majority of 218 votes for it.
House Democrats also must resolve internal disagreements relating to abortion services and health care for immigrants before they can send the bill to the House floor for a vote.
___
Associated Press writers Julie Hirschfeld Davis, Ben Evans, Andrew Miga, Ken Thomas, Erica Werner and Ricardo Alonso-Zaldivar contributed to this report.
Income tax developments. This page provides generalized information and may not apply to you and should not be acted upon without specific professional advice. You should consult your tax adviser if you have any questions.
Tuesday, October 27, 2009
Public Option Push in Senate Comes With Escape Hatch
Sen. Reid's plan is to pay physicians under the public option at Medicare rate. Some doctors have already shunned Medicare patients as they claim Medicare reimbursements do not cover cost, see http://money.cnn.com/2009/10/27/news/economy/healthcare_medicare_doctors/index.htm
http://www.nytimes.com/2009/10/27/health/policy/27health.html
By ROBERT PEAR and DAVID M. HERSZENHORN
Published: October 26, 2009
WASHINGTON — The Senate majority leader, Harry Reid, sided with his party’s liberals on Monday and announced that he would include a government-run insurance plan in health care legislation that he plans to take to the Senate floor within a few weeks.
His proposal came with an escape hatch: A state could refuse to participate in the public insurance plan by adopting a law to opt out. Even so, the announcement was a turning point in the debate over how much of a role government should play in an overhauled health care system, and it set the stage for a test of Democratic party unity.
With Republicans united for now in opposition to any bill including a public option, Mr. Reid needs support from all members of his caucus — 58 Democrats and two independents — to take up the legislation. Aides said Monday that he appeared to be short of that goal, lacking firm commitments from several members of the caucus.
Should Mr. Reid prevail, both houses of Congress would be poised to act on bills including a government-run plan to compete with private insurers in selling health coverage to consumers. The House is still weighing the details of its approach, but Democratic leaders have made clear they will include a government plan in their version of the bill.
Just weeks ago, the prospects for such an approach seemed remote, reflecting all-out opposition from conservatives to what they considered an excessive government role in the economy and a lack of enthusiasm from many moderate Democrats. But the idea has consistently drawn strong support in national polls, and it has backing from President Obama, though he has not insisted on it.
“The best way to move forward is to include a public option with the opt-out provision for states,” said Mr. Reid, Democrat of Nevada. “I believe that a public option can achieve the goal of bringing meaningful reform to our broken system.”
Mr. Reid’s decision was acclaimed by liberal organizations like MoveOn, Families USA and Health Care for America Now, a coalition that includes labor unions and civil rights groups.
But Mr. Reid lost the one Republican who had given Democratic efforts a tinge of bipartisanship, Senator Olympia J. Snowe of Maine. She has proposed a different approach, in which a government plan would become available only if states did not make progress in reducing insurance premiums and covering more of their residents.
“I am deeply disappointed with the majority leader’s decision to include a public option as the focus of the legislation,” Ms. Snowe said. “I still believe that a fallback, safety-net plan, to be triggered and available immediately in states where insurance companies fail to offer plans that meet the standards of affordability, could have been the road toward achieving a broader bipartisan consensus in the Senate.”
Mr. Reid and his aides provided few details of his proposal. They said the public plan would be national in scope and would be available on the first day that major provisions of the health care legislation take effect, in 2013.
The government plan would negotiate payment rates with doctors, hospitals and other health care providers. Some liberal Democrats, including the House speaker, Nancy Pelosi, have said payments should be pegged to Medicare rates, which could save money for the government and for consumers.
The debate over the public option has highlighted a divide among Democrats. The Senate health committee included a public plan in the bill it approved in July. The Senate Finance Committee rejected two versions of the public plan before approving its bill this month.
Those who voted against the public plan on the finance panel included three Democratic senators: Max Baucus of Montana, the committee chairman, and two centrists, Kent Conrad of North Dakota and Blanche Lincoln of Arkansas. Mr. Baucus had said he was open to a public option but did not think it could get 60 votes in the Senate.
As an alternative to a government-run plan, Mr. Conrad has proposed insurance cooperatives: essentially nonprofit, member-run groups, offering coverage to individuals and small groups. Proponents say they could save money by negotiating discounts with health care providers; the Congressional Budget Office sees no significant savings.
Mr. Reid said his plan would include co-ops, as well as the government plan. States that opt out of the public plan could not offer co-ops, an aide to Mr. Reid said.
Liberals see the public option as essential to the success of the legislation, saying it would foster competition and thus help drive down premium costs. With his action on Monday, Mr. Reid showed liberals he was doing all he could to achieve their goal. If his effort falters, he could propose other variations of a public plan, like one with the trigger mechanism Ms. Snowe proposed.
Mr. Reid, who faces a stiff challenge in his re-election bid, said he knew Ms. Snowe “does not like a public option of any kind,” and he held out hope that she would ultimately support the bill.
Pressed on whether he had the needed votes, Mr. Reid said, “I believe we clearly will have the support of my caucus to move to this bill and start legislating.”
A Democrat on Capitol Hill who backs the public option said “there is a lot of concern” that Mr. Reid had made his decision without nailing down the votes to prevail on the Senate floor.
The White House press secretary, Robert Gibbs, said President Obama was pleased with Mr. Reid’s decision. “He supports the public option because it has the potential to play an essential role in holding insurance companies accountable through choice and competition,” Mr. Gibbs said.
Republicans and insurance companies assailed the decision. “No matter what you call it or how you dress it up, the Democrats’ proposal is government-run insurance,” said Senator Jon Kyl of Arizona, the No. 2 Republican in the Senate.
Liberal senators have urged Mr. Reid to include the public option in the bill he is putting together, working with versions approved by two Senate panels.
At a town-hall-style meeting in Colorado in August, Mr. Obama complained that people on the left and the right had become “fixated” on the public plan, which he described as “just one sliver” of efforts to overhaul the health care system.
For the moment, Senate Democratic leaders are taking an aggressive approach, defying Republicans and brushing aside the objections of moderate Democrats who are apprehensive about a public plan. “All the national polls show a wide majority of Americans support the public option,” Mr. Reid said.
But Mr. Reid’s decision will not be the last word. The Senate will probably spend weeks on the health care bill and could vote on dozens of amendments, including several to alter or eliminate his version of a public plan. At any stage, 60 votes could be required.
http://www.nytimes.com/2009/10/27/health/policy/27health.html
By ROBERT PEAR and DAVID M. HERSZENHORN
Published: October 26, 2009
WASHINGTON — The Senate majority leader, Harry Reid, sided with his party’s liberals on Monday and announced that he would include a government-run insurance plan in health care legislation that he plans to take to the Senate floor within a few weeks.
His proposal came with an escape hatch: A state could refuse to participate in the public insurance plan by adopting a law to opt out. Even so, the announcement was a turning point in the debate over how much of a role government should play in an overhauled health care system, and it set the stage for a test of Democratic party unity.
With Republicans united for now in opposition to any bill including a public option, Mr. Reid needs support from all members of his caucus — 58 Democrats and two independents — to take up the legislation. Aides said Monday that he appeared to be short of that goal, lacking firm commitments from several members of the caucus.
Should Mr. Reid prevail, both houses of Congress would be poised to act on bills including a government-run plan to compete with private insurers in selling health coverage to consumers. The House is still weighing the details of its approach, but Democratic leaders have made clear they will include a government plan in their version of the bill.
Just weeks ago, the prospects for such an approach seemed remote, reflecting all-out opposition from conservatives to what they considered an excessive government role in the economy and a lack of enthusiasm from many moderate Democrats. But the idea has consistently drawn strong support in national polls, and it has backing from President Obama, though he has not insisted on it.
“The best way to move forward is to include a public option with the opt-out provision for states,” said Mr. Reid, Democrat of Nevada. “I believe that a public option can achieve the goal of bringing meaningful reform to our broken system.”
Mr. Reid’s decision was acclaimed by liberal organizations like MoveOn, Families USA and Health Care for America Now, a coalition that includes labor unions and civil rights groups.
But Mr. Reid lost the one Republican who had given Democratic efforts a tinge of bipartisanship, Senator Olympia J. Snowe of Maine. She has proposed a different approach, in which a government plan would become available only if states did not make progress in reducing insurance premiums and covering more of their residents.
“I am deeply disappointed with the majority leader’s decision to include a public option as the focus of the legislation,” Ms. Snowe said. “I still believe that a fallback, safety-net plan, to be triggered and available immediately in states where insurance companies fail to offer plans that meet the standards of affordability, could have been the road toward achieving a broader bipartisan consensus in the Senate.”
Mr. Reid and his aides provided few details of his proposal. They said the public plan would be national in scope and would be available on the first day that major provisions of the health care legislation take effect, in 2013.
The government plan would negotiate payment rates with doctors, hospitals and other health care providers. Some liberal Democrats, including the House speaker, Nancy Pelosi, have said payments should be pegged to Medicare rates, which could save money for the government and for consumers.
The debate over the public option has highlighted a divide among Democrats. The Senate health committee included a public plan in the bill it approved in July. The Senate Finance Committee rejected two versions of the public plan before approving its bill this month.
Those who voted against the public plan on the finance panel included three Democratic senators: Max Baucus of Montana, the committee chairman, and two centrists, Kent Conrad of North Dakota and Blanche Lincoln of Arkansas. Mr. Baucus had said he was open to a public option but did not think it could get 60 votes in the Senate.
As an alternative to a government-run plan, Mr. Conrad has proposed insurance cooperatives: essentially nonprofit, member-run groups, offering coverage to individuals and small groups. Proponents say they could save money by negotiating discounts with health care providers; the Congressional Budget Office sees no significant savings.
Mr. Reid said his plan would include co-ops, as well as the government plan. States that opt out of the public plan could not offer co-ops, an aide to Mr. Reid said.
Liberals see the public option as essential to the success of the legislation, saying it would foster competition and thus help drive down premium costs. With his action on Monday, Mr. Reid showed liberals he was doing all he could to achieve their goal. If his effort falters, he could propose other variations of a public plan, like one with the trigger mechanism Ms. Snowe proposed.
Mr. Reid, who faces a stiff challenge in his re-election bid, said he knew Ms. Snowe “does not like a public option of any kind,” and he held out hope that she would ultimately support the bill.
Pressed on whether he had the needed votes, Mr. Reid said, “I believe we clearly will have the support of my caucus to move to this bill and start legislating.”
A Democrat on Capitol Hill who backs the public option said “there is a lot of concern” that Mr. Reid had made his decision without nailing down the votes to prevail on the Senate floor.
The White House press secretary, Robert Gibbs, said President Obama was pleased with Mr. Reid’s decision. “He supports the public option because it has the potential to play an essential role in holding insurance companies accountable through choice and competition,” Mr. Gibbs said.
Republicans and insurance companies assailed the decision. “No matter what you call it or how you dress it up, the Democrats’ proposal is government-run insurance,” said Senator Jon Kyl of Arizona, the No. 2 Republican in the Senate.
Liberal senators have urged Mr. Reid to include the public option in the bill he is putting together, working with versions approved by two Senate panels.
At a town-hall-style meeting in Colorado in August, Mr. Obama complained that people on the left and the right had become “fixated” on the public plan, which he described as “just one sliver” of efforts to overhaul the health care system.
For the moment, Senate Democratic leaders are taking an aggressive approach, defying Republicans and brushing aside the objections of moderate Democrats who are apprehensive about a public plan. “All the national polls show a wide majority of Americans support the public option,” Mr. Reid said.
But Mr. Reid’s decision will not be the last word. The Senate will probably spend weeks on the health care bill and could vote on dozens of amendments, including several to alter or eliminate his version of a public plan. At any stage, 60 votes could be required.
Labels:
health plan
Monday, October 26, 2009
Health care waste and fraud
Here is a 60 Minutes broadcast on Medicare fraud that would make one's blood pressure go up:
http://www.cbsnews.com/video/watch/?id=5419844n
And here is an article about medical waste. The problem is other than eliminating duplicated tests by using electronic records, I really don't see any possible savings. I don't see doctors willing to risk malpractice insurance by ordering fewer tests. I don't see use of ER would reduce as long as we don't have enough primary care physicians. If the government is capable of catching the crooks, they would have done that already, with or without the current proposed health care reforms. What makes anyone think the current proposal would reduce the type of errors cited in this article?
The sad fact is that if we incur $60 billion worth of fraud in Medicare now, as cited by 60 Minutes, expanding that health care system to cover more people with a public option will no doubt increase fraudulent claims.
In my opinion, doctors in the U.S. spend more time on paperwork is because of the need for good documentation. Having good documentations serve two purposes. They provide better patient care and they can be used by the doctors to defend themselves in malpractice lawsuits.
And unless the government takes over the entire health care system, there will be needs for health care providers to continue sending billings.
http://news.yahoo.com/s/nm/20091026/ts_nm/us_usa_healthcare_waste_4
Healthcare system wastes up to $800 billion a year
By Maggie Fox, Health and Science Editor Maggie Fox, Health And Science Editor – 33 mins ago
WASHINGTON (Reuters) – The U.S. healthcare system is just as wasteful as President Barack Obama says it is, and proposed reforms could be paid for by fixing some of the most obvious inefficiencies, preventing mistakes and fighting fraud, according to a Thomson Reuters report released on Monday.
The U.S. healthcare system wastes between $505 billion and $850 billion every year, the report from Robert Kelley, vice president of healthcare analytics at Thomson Reuters, found.
"America's healthcare system is indeed hemorrhaging billions of dollars, and the opportunities to slow the fiscal bleeding are substantial," the report reads.
"The bad news is that an estimated $700 billion is wasted annually. That's one-third of the nation's healthcare bill," Kelley said in a statement.
"The good news is that by attacking waste we can reduce healthcare costs without adversely affecting the quality of care or access to care."
One example -- a paper-based system that discourages sharing of medical records accounts for 6 percent of annual overspending.
"It is waste when caregivers duplicate tests because results recorded in a patient's record with one provider are not available to another or when medical staff provides inappropriate treatment because relevant history of previous treatment cannot be accessed," the report reads.
Some other findings in the report from Thomson Reuters, the parent company of Reuters:
"American physicians spend nearly eight hours per week on paperwork and employ 1.66 clerical workers per doctor, far more than in Canada," it says, quoting a 2003 New England Journal of Medicine paper by Harvard University researcher Dr. Steffie Woolhandler.
Yet primary care doctors are lacking, forcing wasteful use of emergency rooms, for instance, the report reads.
All this could help explain why Americans spend more per capita and the highest percentage of GDP on healthcare than any other OECD country, yet has an unhealthier population with more diabetes, obesity and heart disease and higher rates of neonatal deaths than other developed nations.
Democratic Senator Charles Schumer said on Sunday that Senate Democratic leaders are close to securing enough votes to pass legislation to start reform of the country's $2.5 trillion healthcare system.
__________
Also see http://guywong.blogspot.com/2009/11/10-ways-to-cut-health-care-costs-right.html
http://www.cbsnews.com/video/watch/?id=5419844n
And here is an article about medical waste. The problem is other than eliminating duplicated tests by using electronic records, I really don't see any possible savings. I don't see doctors willing to risk malpractice insurance by ordering fewer tests. I don't see use of ER would reduce as long as we don't have enough primary care physicians. If the government is capable of catching the crooks, they would have done that already, with or without the current proposed health care reforms. What makes anyone think the current proposal would reduce the type of errors cited in this article?
The sad fact is that if we incur $60 billion worth of fraud in Medicare now, as cited by 60 Minutes, expanding that health care system to cover more people with a public option will no doubt increase fraudulent claims.
In my opinion, doctors in the U.S. spend more time on paperwork is because of the need for good documentation. Having good documentations serve two purposes. They provide better patient care and they can be used by the doctors to defend themselves in malpractice lawsuits.
And unless the government takes over the entire health care system, there will be needs for health care providers to continue sending billings.
http://news.yahoo.com/s/nm/20091026/ts_nm/us_usa_healthcare_waste_4
Healthcare system wastes up to $800 billion a year
By Maggie Fox, Health and Science Editor Maggie Fox, Health And Science Editor – 33 mins ago
WASHINGTON (Reuters) – The U.S. healthcare system is just as wasteful as President Barack Obama says it is, and proposed reforms could be paid for by fixing some of the most obvious inefficiencies, preventing mistakes and fighting fraud, according to a Thomson Reuters report released on Monday.
The U.S. healthcare system wastes between $505 billion and $850 billion every year, the report from Robert Kelley, vice president of healthcare analytics at Thomson Reuters, found.
"America's healthcare system is indeed hemorrhaging billions of dollars, and the opportunities to slow the fiscal bleeding are substantial," the report reads.
"The bad news is that an estimated $700 billion is wasted annually. That's one-third of the nation's healthcare bill," Kelley said in a statement.
"The good news is that by attacking waste we can reduce healthcare costs without adversely affecting the quality of care or access to care."
One example -- a paper-based system that discourages sharing of medical records accounts for 6 percent of annual overspending.
"It is waste when caregivers duplicate tests because results recorded in a patient's record with one provider are not available to another or when medical staff provides inappropriate treatment because relevant history of previous treatment cannot be accessed," the report reads.
Some other findings in the report from Thomson Reuters, the parent company of Reuters:
- Unnecessary care such as the overuse of antibiotics and lab tests to protect against malpractice exposure makes up 37 percent of healthcare waste or $200 to $300 billion a year.
- Fraud makes up 22 percent of healthcare waste, or up to $200 billion a year in fraudulent Medicare claims, kickbacks for referrals for unnecessary services and other scams.
- Administrative inefficiency and redundant paperwork account for 18 percent of healthcare waste.
- Medical mistakes account for $50 billion to $100 billion in unnecessary spending each year, or 11 percent of the total.
- Preventable conditions such as uncontrolled diabetes cost $30 billion to $50 billion a year.
"American physicians spend nearly eight hours per week on paperwork and employ 1.66 clerical workers per doctor, far more than in Canada," it says, quoting a 2003 New England Journal of Medicine paper by Harvard University researcher Dr. Steffie Woolhandler.
Yet primary care doctors are lacking, forcing wasteful use of emergency rooms, for instance, the report reads.
All this could help explain why Americans spend more per capita and the highest percentage of GDP on healthcare than any other OECD country, yet has an unhealthier population with more diabetes, obesity and heart disease and higher rates of neonatal deaths than other developed nations.
Democratic Senator Charles Schumer said on Sunday that Senate Democratic leaders are close to securing enough votes to pass legislation to start reform of the country's $2.5 trillion healthcare system.
__________
Also see http://guywong.blogspot.com/2009/11/10-ways-to-cut-health-care-costs-right.html
Labels:
health plan
Sunday, October 25, 2009
Health care issues: How the US system evolved
http://www3.signonsandiego.com/stories/2009/oct/20/us-health-care-briefing-102009/?nation
By The Associated Press
6:30 a.m. October 20, 2009
A look at key issues in the health care debate:
THE ISSUE: Why is the United States the only wealthy industrialized nation that does not have universal health coverage?
THE POLITICS: Health insurance in the United States is provided primarily by employers. The government picks up coverage for retirees and the disabled through Medicare, for the poor through Medicaid, and for military veterans and members of Indian tribes. That still leaves many people without coverage, estimated at 40 to 50 million. The U.S. system was shaped by a World War II government policy that imposed wage controls when much of the nation's work force was off at war. Barred from wage increases, employers turned to health insurance benefits to attract workers, and job-related health benefits became a staple in the postwar years. President Barack Obama takes note of the patchwork nature of the U.S. health care system, but argues it's politically impossible to throw out the entire system and start from scratch.
WHAT IT MEANS: Any overhaul of the U.S. system will be built on a foundation of employer-provided health care. Industrialized countries that provide universal coverage do so because those systems evolved from their own unique histories. Britain, for example, found it necessary to provide government-run care to its military and civilians alike when it came under attack in World War II, and that gave rise to its current, largely government-owned, system. France's care is built on a long-standing system of employer- and union-sponsored payroll tax insurance funds that were expanded over the years.
– Jim Drinkard
By The Associated Press
6:30 a.m. October 20, 2009
A look at key issues in the health care debate:
THE ISSUE: Why is the United States the only wealthy industrialized nation that does not have universal health coverage?
THE POLITICS: Health insurance in the United States is provided primarily by employers. The government picks up coverage for retirees and the disabled through Medicare, for the poor through Medicaid, and for military veterans and members of Indian tribes. That still leaves many people without coverage, estimated at 40 to 50 million. The U.S. system was shaped by a World War II government policy that imposed wage controls when much of the nation's work force was off at war. Barred from wage increases, employers turned to health insurance benefits to attract workers, and job-related health benefits became a staple in the postwar years. President Barack Obama takes note of the patchwork nature of the U.S. health care system, but argues it's politically impossible to throw out the entire system and start from scratch.
WHAT IT MEANS: Any overhaul of the U.S. system will be built on a foundation of employer-provided health care. Industrialized countries that provide universal coverage do so because those systems evolved from their own unique histories. Britain, for example, found it necessary to provide government-run care to its military and civilians alike when it came under attack in World War II, and that gave rise to its current, largely government-owned, system. France's care is built on a long-standing system of employer- and union-sponsored payroll tax insurance funds that were expanded over the years.
– Jim Drinkard
Labels:
health plan
Health Bills In Congress Won't Fix Doctor Shortage
http://www.kaiserhealthnews.org/Stories/2009/October/12/primary-care-doctor-shortage.aspx
By Phil Galewitz, KHN Staff Writer
Oct 12, 2009
Even as Congress moves to expand health insurance coverage to millions of Americans, it's doing little to ensure there will be enough primary care doctors to meet the expected surge in demand for treatment, experts say.
The American Academy of Family Physicians predicts that the shortage of family doctors will reach 40,000 in the next 10 years, as medical schools send about half the needed number of graduates into primary care medicine. The overall shortage of doctors is expected to grow to nearly 160,000 by 2025, according to the Association of American Medical Colleges.
“I don't see anything in the legislation that will greatly increase the primary care pipeline," said Dr. Russell Robertson, chairman of the Council on Graduate Medical Education, which advises Congress. In addition to making sure patients have access to care, increasing the number and proportion of primary care doctors is crucial to lowering health costs, he said. Primary care doctors make up about a third of all physicians, though in most industrialized nations they make up half.
"We can't bend the cost curve without increasing primary care providers," said Robertson, who is also chair of family and community medicine at Northwestern University's Feinberg School of Medicine in Chicago.
Add More Residents? 'Dead on Arrival'
Almost everyone agrees on how to build up the supply of primary care physicians: create more residency positions at teaching hospitals for family doctors and internists to complete their training and significantly increase how much primary care doctors get paid by Medicare and other insurers. But there’s resistance to these steps because of their costs.
A proposal backed by Senate Majority Leader Harry Reid, D-Nev., and the teaching hospital lobby to add 15,000 Medicare-funded medical residency positions -- a 15 percent increase that would favor more primary care training -- was considered dead on arrival because of its $10 billion price tag over a decade. Proponents said it was a small price to pay, in legislation that could run as high as $1 trillion, to ensure that patients have access to doctors.
Instead, the House and Senate overhaul bills would redistribute about 1,000 unfilled residency positions to teaching hospitals that commit to creating more primary care residencies. The Senate Finance Committee bill would give 15 mostly southern and western states preference for those positions because they have a high proportion of doctor shortages or a low percentage of medical residents. Ten of these states have representatives on the Finance Committee.
Proposals to significantly increase Medicare payments for primary care doctors have gone nowhere in part because the money would come from payments to higher-paid specialists — who, not surprisingly, oppose a pay cut.
As they now stand, the House and Senate overhaul bills call for a 10 percent bonus for primary care doctors for five years, an increase in Medicare payment rates that most experts say would have only a slight impact on encouraging new doctors to go into primary care careers. Family doctors on average make about $173,000, less than half of what specialists such as cardiologists earn, according to physician recruiters Merritt Hawkins & Associates.
Dr. Darrell Kirch, CEO of the Association of American Medical Colleges, said the extra training slots emanating from the redistribution of unfilled residency position would amount to a “drop in the bucket.” Kirch noted that after Massachusetts in 2006 required residents to have health insurance, the demand for care quickly overwhelmed the state's doctors. "It’s a huge issue that concerns us greatly," said Kirch, whose association represents all 130 medical schools and nearly 400 major teaching hospitals.
Money Goes To Specialist Training
Dr. Ted Epperly, a Boise, Idaho, family doctor who is president of the American Academy of Family Physicians, said family doctors would need about a 30 percent increase in pay to encourage more young physicians to enter primary care. "The bills are anemic,” he said, “but at least a step in the right direction.”
Some medical workforce experts applaud Congress for trying to target how it spends billions in medical education funds to help states with the biggest needs and to promote primary care over specialty care. “It's good to see Congress for the first time step to the plate to work on rebalancing the physician supply," said Dr. Mark Kelley, executive vice president of the Henry Ford Health System in Detroit and member of the Council on Graduate Medical Education. But like Kirch, Kelley said the redistribution of 1,000 residency slots will only make a small dent in the shortage problem.
The number of residency training positions for all doctors has been flat for years. That's because in a budget-cutting move in 1997, Congress froze the number of Medicare-funded medical residency positions. Since then, the U.S. population has increased by more than 30 million – making the need for additional medical residents particularly acute, according to the Association of American Medical Colleges. While some teaching hospitals have added residency positions using their own money, those slots have largely gone to train specialists who can improve the facilities' bottom line.
Obama administration officials say the Democratic health bills are doing more than paying lip service to the physician workforce issues. An official from the Health and Human Services Office of Health Reform said the 10 percent bonus to primary care doctors, additional loans and scholarships and a medical home pilot project will all help. In the medical home pilot, primary care doctors get paid extra money to coordinate care to the patients.
The bills would also increase funding to the National Health Service Corps, where primary care doctors can get up to $50,000 to help repay loans in exchange for working two to four years in a federally-designated physician shortage area.
Whatever the impact of those measures, they don't address the main issue raised by experts such as Ken Raske, president of the Greater New York Hospital Association. Giving millions of Americans health insurance, while not increasing the doctor supply is a recipe for trouble in his view. "Providing a benefit that you can't deliver the product on will be a real problem," he said. "Without expanding the number of residency slots you are not increasing the pipeline."
__________
This article also appeared on the National Public Radio web site:
http://www.npr.org/templates/story/story.php?storyId=113728158&ft=1&f=106181748
By Phil Galewitz, KHN Staff Writer
Oct 12, 2009
Even as Congress moves to expand health insurance coverage to millions of Americans, it's doing little to ensure there will be enough primary care doctors to meet the expected surge in demand for treatment, experts say.
The American Academy of Family Physicians predicts that the shortage of family doctors will reach 40,000 in the next 10 years, as medical schools send about half the needed number of graduates into primary care medicine. The overall shortage of doctors is expected to grow to nearly 160,000 by 2025, according to the Association of American Medical Colleges.
“I don't see anything in the legislation that will greatly increase the primary care pipeline," said Dr. Russell Robertson, chairman of the Council on Graduate Medical Education, which advises Congress. In addition to making sure patients have access to care, increasing the number and proportion of primary care doctors is crucial to lowering health costs, he said. Primary care doctors make up about a third of all physicians, though in most industrialized nations they make up half.
"We can't bend the cost curve without increasing primary care providers," said Robertson, who is also chair of family and community medicine at Northwestern University's Feinberg School of Medicine in Chicago.
Add More Residents? 'Dead on Arrival'
Almost everyone agrees on how to build up the supply of primary care physicians: create more residency positions at teaching hospitals for family doctors and internists to complete their training and significantly increase how much primary care doctors get paid by Medicare and other insurers. But there’s resistance to these steps because of their costs.
A proposal backed by Senate Majority Leader Harry Reid, D-Nev., and the teaching hospital lobby to add 15,000 Medicare-funded medical residency positions -- a 15 percent increase that would favor more primary care training -- was considered dead on arrival because of its $10 billion price tag over a decade. Proponents said it was a small price to pay, in legislation that could run as high as $1 trillion, to ensure that patients have access to doctors.
Instead, the House and Senate overhaul bills would redistribute about 1,000 unfilled residency positions to teaching hospitals that commit to creating more primary care residencies. The Senate Finance Committee bill would give 15 mostly southern and western states preference for those positions because they have a high proportion of doctor shortages or a low percentage of medical residents. Ten of these states have representatives on the Finance Committee.
Proposals to significantly increase Medicare payments for primary care doctors have gone nowhere in part because the money would come from payments to higher-paid specialists — who, not surprisingly, oppose a pay cut.
As they now stand, the House and Senate overhaul bills call for a 10 percent bonus for primary care doctors for five years, an increase in Medicare payment rates that most experts say would have only a slight impact on encouraging new doctors to go into primary care careers. Family doctors on average make about $173,000, less than half of what specialists such as cardiologists earn, according to physician recruiters Merritt Hawkins & Associates.
Dr. Darrell Kirch, CEO of the Association of American Medical Colleges, said the extra training slots emanating from the redistribution of unfilled residency position would amount to a “drop in the bucket.” Kirch noted that after Massachusetts in 2006 required residents to have health insurance, the demand for care quickly overwhelmed the state's doctors. "It’s a huge issue that concerns us greatly," said Kirch, whose association represents all 130 medical schools and nearly 400 major teaching hospitals.
Money Goes To Specialist Training
Dr. Ted Epperly, a Boise, Idaho, family doctor who is president of the American Academy of Family Physicians, said family doctors would need about a 30 percent increase in pay to encourage more young physicians to enter primary care. "The bills are anemic,” he said, “but at least a step in the right direction.”
Some medical workforce experts applaud Congress for trying to target how it spends billions in medical education funds to help states with the biggest needs and to promote primary care over specialty care. “It's good to see Congress for the first time step to the plate to work on rebalancing the physician supply," said Dr. Mark Kelley, executive vice president of the Henry Ford Health System in Detroit and member of the Council on Graduate Medical Education. But like Kirch, Kelley said the redistribution of 1,000 residency slots will only make a small dent in the shortage problem.
The number of residency training positions for all doctors has been flat for years. That's because in a budget-cutting move in 1997, Congress froze the number of Medicare-funded medical residency positions. Since then, the U.S. population has increased by more than 30 million – making the need for additional medical residents particularly acute, according to the Association of American Medical Colleges. While some teaching hospitals have added residency positions using their own money, those slots have largely gone to train specialists who can improve the facilities' bottom line.
Obama administration officials say the Democratic health bills are doing more than paying lip service to the physician workforce issues. An official from the Health and Human Services Office of Health Reform said the 10 percent bonus to primary care doctors, additional loans and scholarships and a medical home pilot project will all help. In the medical home pilot, primary care doctors get paid extra money to coordinate care to the patients.
The bills would also increase funding to the National Health Service Corps, where primary care doctors can get up to $50,000 to help repay loans in exchange for working two to four years in a federally-designated physician shortage area.
Whatever the impact of those measures, they don't address the main issue raised by experts such as Ken Raske, president of the Greater New York Hospital Association. Giving millions of Americans health insurance, while not increasing the doctor supply is a recipe for trouble in his view. "Providing a benefit that you can't deliver the product on will be a real problem," he said. "Without expanding the number of residency slots you are not increasing the pipeline."
__________
This article also appeared on the National Public Radio web site:
http://www.npr.org/templates/story/story.php?storyId=113728158&ft=1&f=106181748
Labels:
health plan
Saturday, October 24, 2009
Bank failures stack up: Now 106 for 2009

http://money.cnn.com/2009/10/23/news/economy/bank_failure/index.htm
Banks in Florida, Georgia, Illinois, Minnesota and Wisconsin, were shuttered, costing the FDIC an estimated $356.6 million.
By Julianne Pepitone, CNNMoney.com staff reporter
Last Updated: October 23, 2009: 8:14 PM ET
NEW YORK (CNNMoney.com) -- The tally of bank failures easily broke past the No. 100 milestone on Friday night, with regulators announcing the year's 106th closure.
That's more than four times the number that were closed in 2008, and the highest total since 1992, when 181 banks failed.
Earlier on Friday evening the dubious honor of the 100th failure went to Partners Bank, of Naples, Fla., which had $65.5 million in assets, according to the Federal Deposit Insurance Corp.
The 101st failure was American United Bank, of Lawrenceville, Ga., which had $111 million in assets.
The 102nd failure was another Naples, Fla., institution: Hillcrest Bank Florida, which had $83 million in assets.
The 103rd closure was Bradenton, Fla.-based Flagship National Bank, with $190 million in assets.
The 104th was Bank of Elmwood, based in Racine, Wis., which had $327.4 million in assets.
The 105th failure was Riverview Community Bank of Otsego, Minn., with $108 million in assets.
The 106th failure was First Dupage Bank in Westmont, Ill., which had $279 million in assets.
Customers of all seven banks are protected, however. The Federal Deposit Insurance Corp., which has insured bank deposits since the Great Depression, covers customer accounts up to $250,000. This is funded through premiums paid by member banks.
In fact, to reassure borrowers, FDIC chair Sheila Bair posted a video message to the agency's Web site, saying "for the insured depositor, a bank failure is a non-event."
Still, Bair cautioned that "until the healing process is complete, there will be more bank failures."
What happens to the banks. Fort Lauderdale, Fla.-based Stonegate Bank will assume control of all Partners Bank's $64.9 million in deposits. It will also take over Hillcrest Bank's $84 million in deposits. The two branches of Partners Bank and six branches of Hillcrest will reopen on Monday as branches of Stonegate.
Moultrie, Ga.-based Ameris Bank will pay the FDIC a premium of 1.02% to take control of American United's $101 million in deposits. The FDIC and Ameris Bank entered into a loss-share transaction on $92 million of American United's assets, an agreement in which Ameris will share in the losses on the assets covered.
The single branch of American United Bank will reopen on Monday as a branch of Ameris.
Lake City, Fla.-based First Federal Bank will take over all of Flagship National Bank's $175 million in deposits. The four branches of Flagship will reopen Monday as branches of First Federal.
Bank of Elmwood's $273.2 million in deposits are now controlled by Tri City National Bank, based in Oak Creek, Wis. The five branches of Bank of Elmwood will reopen on Saturday as branches of Tri City.
Stillwater, Minn.-based Central Bank will take control of Riverview Community Bank's $80 million in deposits. The FDIC and Central Bank entered into a loss-share transaction on $75 million of Riverview's assets.
First Dupage Bank's $254 million in deposits are now being handled by First Midwest Bank of Itasca, Ill. The FDIC and First Midwest Bank entered into a loss-share transaction on approximately $247 million of First Dupage Bank's assets. The sole First Dupage branch will reopn Saturday as an outpost of First Midwest.
The failure of the six banks will cost the Deposit Insurance Fund an estimated $356.6 million, according to the FDIC.
Why regional banks are failing. While larger financial institutions have received aid from the federal government, smaller banks have found themselves left adrift. Like their larger counterparts, many of these banks made risky loans to individuals and real estate developers during the boom years and are now facing large numbers of defaults as the recession drags on.
Rising unemployment has made it difficult for many individuals to keep up with expenses, and businesses are feeling the crunch of consumers' reduced spending power. As a result, regional banks are left holding loans their customers can't repay.
Problem banks list looms. The FDIC keeps a list of "problem banks," though it does not disclose the names to the general public out of fear that depositors at those institutions may prompt a "run on the bank."
In June, the agency said 416 banks were at risk of failure -- the highest level in 15 years.
It's a whopping figure, to be sure. But even as the pace of failures accelerates, 2009's numbers remain far from what happened during the savings and loan crisis two decades ago. More than 1,900 financial institutions failed from 1987-1991, peaking at 534 closures in 1989.
Federal coffers running dry. An average of 10 banks have failed per month this year, and the federal coffer is thinning under the massive strain. The fund now stands at $7.5 billion, down significantly from $45 billion a year ago.
When the FDIC factors in expected closures, the agency says the fund is in the red and will likely remain there through 2012. Bank failure costs are expected to total $100 billion over the next four years, leaving regulators strapped for cash.
Last month, the FDIC discussed how to raise quick cash to replenish the fund. The agency proposed that banks prepay their deposit insurance premiums for the next three years. To top of page
First Published: October 23, 2009: 5:40 PM ET
__________
For an interactive map, see http://money.cnn.com/news/storysupplement/economy/bank_failures/index.htm
Labels:
banks failure
Friday, October 23, 2009
Bank failures hit 100 for year

http://www.marketwatch.com/story/bank-failures-hit-100-for-year-2009-10-23
By Greg Morcroft, MarketWatch
NEW YORK (MarketWatch) -- A Naples, Fla., bank failed Friday, marking the first year since 1992 that at least 100 have gone under
Experts suggest we could be no more than 10% of the way through this cycle of bank collapses, which is sure to be the worst run of closures since the Great Depression.
The parade of bank failures continued on Friday as the FDIC took control of Partners Bank of Naples after it was closed by the Office of Thrift Supervision. See http://www.marketwatch.com/story/california-bank-99th-to-fail-in-us-in-2009-2009-10-16.
So far 100 banks have failed in 2009. See FDIC timeline of 2009's failed banks.
CreditSights, which tracks the dismal data, predicts that in the current cycle, from 2008 through 2011, as many as 1,100 banks will fail. That would wipe out 13.4% of all U.S. banks, representing 7% of U.S. banking assets.
The last year in which the FDIC had that many banks to deal with was in 1992, at the tail end of the last real estate crisis. The FDIC rescued 122 in 1992, according to Keefe, Bruyette & Woods researchers.
The increasing stream of bank failures is likely to run through 2011 according to some industry experts, as the fallout from the credit crisis continues.
The panic that started in 2007 as a credit crisis quickly morphed into a full blown residential real estate collapse. The problems blossomed as prices on mortgage securities backed by ill-conceived loans then collapsed, triggering capital destruction at banks and a fear among firms to lend to each other.
The crisis worsened as tighter credit forced firms to lay off millions of workers, hitting retailers hard and triggering further spikes in credit card and mortgage defaults.
Most of the high profile large banks likely to fail already have, and the backlog of troubled banks now is concentrated at the regional and community level, and is weighed down by commercial real estate and construction loans.
Many smaller banks gorged on commercial real estate lending in the go-go 2000s, amid low interest rates and rising property values.
The fallout has been fast, and furious.
CreditSights' data show that commercial real estate loans made up almost half of all loans at most (80%) of the banks the research firm identified as troubled.
"Another wave of prolonged losses driven by weakness in commercial real estate could prove catastrophic to many of these weakened banks," CreditSights said.
FDIC-insured institutions have set aside just over $338 billion in provisions for loan losses during the past six quarters, an amount that is about four times larger than their provisions during the prior six quarter period, FDIC data show.
"While banks and thrifts are now well along in the process of loss recognition and balance sheet repair, the process will continue well into next year, especially for commercial real estate," FDIC chief Sheila Bair told Congress last week.
As a result, she said, the number of problem institutions increased significantly, to more than 400 during the second quarter.
Now, with unemployment near 10% and credit card default rates about the same, prime mortgage delinquencies are rising, stoking worries among the nation's banks that despite rising stock markets, fundamental banking industry health remains elusive.
Hundreds of billions of dollars of government support is helping to keep the biggest banks afloat, but many of the nation's smaller regional and community banks face failure.
"We expect the numbers of problem institutions to increase and bank failures to remain high for the next several quarters," Bair said.
That's created a devilishly vexing issue for the FDIC, the federal agency charged with making depositors whole.
10% of U.S. banks could fail
Before Friday's bank failures, the year-to-date total assets of the failed banks was $107.14 billion.
By comparison, the nation's four largest banks, excluding former investment banks Morgan Stanley and Goldman Sachs, Bank of America, J.P. Morgan Chase, Citigroup and Wells Fargo, have average annual revenue of about $100 billion.
By contrast, according to the FDIC, during the Great Depression, about 9,100 banks failed between 1931 and 1934 representing a full one-third of the nation's then total banking system.
In modern times, the savings and loan crisis of the late 1980s and early 1990s, defined by the years 1988 through 1992, saw 818 banks, or just under 5% of the industry at the time. The 1988-1992 periods saw 4.4% of the banking industry's assets lost, according to data from CreditSights and the FDIC.
As in all crises, some areas fare worse than others for various reasons.
In this cycle, Georgia has been hit hardest, with 19 failures, followed by Illinois with 16, and California with 10.
By CreditSights estimates, Georgia, Florida and Illinois have the most potentially troubled banks among the states, followed by banks, followed by Texas, Minnesota, Washington State and California.
But if there is a bright side, it's that some of the nation's well-managed smaller banks stand to benefit from picking up assets on the cheap.
"We continue to believe a select group of regional banks with sufficient capital, credit quality, and management talent stand to benefit by expanding their banking franchise through either rolling up failed institutions or acquiring market share and/or key lenders from the dislocation," analysts at Keefe Bruyette & Woods said earlier this month. See story about how regional banks are taking advantage of competitors' failures.
FDIC faces tough calls
The FDIC is facing its own money issues, as its Deposit Insurance Fund, which it uses to pay depositors' claims, fell to just $10.4 billion at the end of the second quarter. The FDIC estimates that its total cost for the 98 bank closings through Friday at $26.44 billion.
The problem the FDIC faces is that none of its options to raise money to fund its Deposit Insurance Fund are too appealing.
On the one hand, the FDIC has already hit banks with a special assessment earlier this year to beef up the fund, but that's not nearly enough to fill the expected void.
Also earlier this year, the agency's board approved a proposal to have the nation's banks prepay 3 three years of insurance premiums, but that too is unlikely to fill the gap the fund faces under CreditSights worst-case scenario.
And, while the FDIC could tap an emergency $500 billion line of credit from the U.S. Treasury, the agency appears loathe to do that given the likely political backlash.
"In the FDIC's view, requiring that institutions prepay assessments is also preferable to borrowing from the U.S. Treasury. Prepayment of assessments ensures that the deposit insurance system remains directly industry-funded and it preserves Treasury borrowing for emergency situations," FDIC chair Sheila Bair told Congress in last week's testimony. See Bair's full testimony.
"Additionally," she added, "the FDIC believes that, unlike borrowing from the Treasury or the FFB, requiring prepaid assessments would not count toward the public debt limit."
CreditSights' analysts agreed that a Treasury deal could prove politically tricky, and the debate sure to surround it could actually prolong the crisis,
"A request to draw down on the Treasury line may become yet another political football pitting banking interests versus small business interests. These types of debates seem to have in the past delayed regulatory action and this could be the case as well with an undercapitalized FDIC," the firm said.
Greg Morcroft is MarketWatch's financial editor in New York.
Labels:
banks failure
Wednesday, October 21, 2009
Senate Rejects ‘Doc Fix’ Spending Bill
http://prescriptions.blogs.nytimes.com/2009/10/21/senate-rejects-doc-fix-spending-bill-as-some-democrats-side-with-republicans/?8au&emc=au
Some Democrats Side With Republicans
By David M. Herszenhorn AND Robert Pear
In a vote that was a highly symbolic proxy for the larger partisan fight over health care policy, the Senate on Wednesday rejected a bill that would have averted steep cuts in Medicare payments to doctors.
Senate Democratic leaders had pushed the bill, which would have cost $247 billion over 10 years, as a standalone measure separate from the broader health care legislation that is President Obama’s top domestic priority.
The bill was meant to fix a longstanding payment formula that calls for annual cuts in Medicare payments to doctors — cuts that for years Congress has avoided with yearly stop-gap measures that have come to be known on Capitol Hill as the “doc fix.”
The Senate majority leader, Harry Reid of Nevada, had argued that flawed doctor payment formula was a longstanding problem and that the cost of fixing it should not count in the price tag of the big health care bill.
The American Medical Association had also lobbied heavily in favor of a permanent correction of the formula, which calls for a 21.5 percent cut in Medicare fees in 2010 and cuts of about 5 percent in each of the next few years.
But Republicans seized on the proposal to suggest that Democrats were not being fully forthcoming about the cost of the broader health care overhaul, which Mr. Obama has said should be about $900 billion and not add to the federal deficits.
And in the end, a dozen Democrats and one independent joined all 40 Senate Republicans in opposing the measure, which failed on a procedural vote by 53 to 47. Under Senate rules, the measure needed 60 votes to advance.
Because Democrats did not propose offsetting the cost of fixing the doctor-payment formula, the bill would have added the full cost of $247 billion to future deficits.
The Senate Republican leader, Mitch McConnell of Kentucky, said that Wednesday’s vote represented a first signal of bipartisan opposition to the Democrats’ larger health care proposals.
“In the Senate’s first vote on health care spending this year, a bipartisan majority rejected the Democrat leadership’s attempt to add another quarter trillion dollars to the national credit card without any plan to pay for it,” Mr. McConnell said in a statement. “With a record deficit and a ballooning national debt, the American people are saying enough is enough. Today’s vote shows that this message is finally starting to get through to Congress. Hopefully it’s a sign of things to come in the health care debate ahead.”
Mr. Reid and other Democrats criticized the Republicans for opposing an adjustment to the doctor-payment formula and accused them of playing politics and simply seeking to obstruct Mr. Obama’s agenda.
The Senate Finance Committee had proposed a one-year fix for the doctor-payment formula as part of the broad health care legislation it approved last week — a proposal that is still being melded with a health care bill passed last summer by the Senate health committee.
And Senator Kent Conrad, Democrat of North Dakota and chairman of the Budget Committee, who was a leading architect of the Senate Finance Committee bill, had proposed a commission to come up with a long-term solution to the Medicare doctor-payment formula and several other recurring budgetary problems.
Mr. Conrad was among the Democrats who voted against the party leadership. Others were Evan Bayh of Indiana, Russ Feingold of Wisconsin, Claire McCaskill of Missouri and Ron Wyden of Oregon.
House Democrats included a permanent adjustment of the doctor payment formula in their health care legislation, at a cost of $228.5 billion over 10 years. But they, too, have said the cost should not count in judging whether the broader health legislation meets Mr. Obama’s requirement of not adding to the deficit.
Since 2003, Congress has stepped in to postpone cuts under the payment formula, in legislation but has usually found ways to offset the cost to the government.
Aides to Mr. Reid said they had no choice but to try to fix the doctor payment formula ahead of debate on the larger health care legislation. Otherwise, they said, an amendment would be offered on the Senate floor to add the formula adjustment to the bill, pushing the overall price-tag of the legislation above $1 trillion and seriously imperiling its chances.
__________
For more on "doc fix", see this editorial in today's Wall Street Journal, "The Doctor Fix Is In":
http://online.wsj.com/article/SB10001424052748704500604574483531025733584.html
Some Democrats Side With Republicans
By David M. Herszenhorn AND Robert Pear
In a vote that was a highly symbolic proxy for the larger partisan fight over health care policy, the Senate on Wednesday rejected a bill that would have averted steep cuts in Medicare payments to doctors.
Senate Democratic leaders had pushed the bill, which would have cost $247 billion over 10 years, as a standalone measure separate from the broader health care legislation that is President Obama’s top domestic priority.
The bill was meant to fix a longstanding payment formula that calls for annual cuts in Medicare payments to doctors — cuts that for years Congress has avoided with yearly stop-gap measures that have come to be known on Capitol Hill as the “doc fix.”
The Senate majority leader, Harry Reid of Nevada, had argued that flawed doctor payment formula was a longstanding problem and that the cost of fixing it should not count in the price tag of the big health care bill.
The American Medical Association had also lobbied heavily in favor of a permanent correction of the formula, which calls for a 21.5 percent cut in Medicare fees in 2010 and cuts of about 5 percent in each of the next few years.
But Republicans seized on the proposal to suggest that Democrats were not being fully forthcoming about the cost of the broader health care overhaul, which Mr. Obama has said should be about $900 billion and not add to the federal deficits.
And in the end, a dozen Democrats and one independent joined all 40 Senate Republicans in opposing the measure, which failed on a procedural vote by 53 to 47. Under Senate rules, the measure needed 60 votes to advance.
Because Democrats did not propose offsetting the cost of fixing the doctor-payment formula, the bill would have added the full cost of $247 billion to future deficits.
The Senate Republican leader, Mitch McConnell of Kentucky, said that Wednesday’s vote represented a first signal of bipartisan opposition to the Democrats’ larger health care proposals.
“In the Senate’s first vote on health care spending this year, a bipartisan majority rejected the Democrat leadership’s attempt to add another quarter trillion dollars to the national credit card without any plan to pay for it,” Mr. McConnell said in a statement. “With a record deficit and a ballooning national debt, the American people are saying enough is enough. Today’s vote shows that this message is finally starting to get through to Congress. Hopefully it’s a sign of things to come in the health care debate ahead.”
Mr. Reid and other Democrats criticized the Republicans for opposing an adjustment to the doctor-payment formula and accused them of playing politics and simply seeking to obstruct Mr. Obama’s agenda.
The Senate Finance Committee had proposed a one-year fix for the doctor-payment formula as part of the broad health care legislation it approved last week — a proposal that is still being melded with a health care bill passed last summer by the Senate health committee.
And Senator Kent Conrad, Democrat of North Dakota and chairman of the Budget Committee, who was a leading architect of the Senate Finance Committee bill, had proposed a commission to come up with a long-term solution to the Medicare doctor-payment formula and several other recurring budgetary problems.
Mr. Conrad was among the Democrats who voted against the party leadership. Others were Evan Bayh of Indiana, Russ Feingold of Wisconsin, Claire McCaskill of Missouri and Ron Wyden of Oregon.
House Democrats included a permanent adjustment of the doctor payment formula in their health care legislation, at a cost of $228.5 billion over 10 years. But they, too, have said the cost should not count in judging whether the broader health legislation meets Mr. Obama’s requirement of not adding to the deficit.
Since 2003, Congress has stepped in to postpone cuts under the payment formula, in legislation but has usually found ways to offset the cost to the government.
Aides to Mr. Reid said they had no choice but to try to fix the doctor payment formula ahead of debate on the larger health care legislation. Otherwise, they said, an amendment would be offered on the Senate floor to add the formula adjustment to the bill, pushing the overall price-tag of the legislation above $1 trillion and seriously imperiling its chances.
__________
For more on "doc fix", see this editorial in today's Wall Street Journal, "The Doctor Fix Is In":
http://online.wsj.com/article/SB10001424052748704500604574483531025733584.html
Labels:
health plan
Tuesday, October 20, 2009
Monday, October 19, 2009
ObamaCare's Tax on Work
http://online.wsj.com/article/SB10001424052748704322004574477401457898882.html
Middle-income families will face a big marginal rate increase.
None of the new distortions that the Senate health-care bill will layer onto the already-distorted tax code have received the attention they deserve, but in particular its effects on marginal tax rates could use scrutiny. Incredibly, for those with lower incomes, ObamaCare will impose a penalty as high as 34% on . . . work.
Central to Max Baucus's plan—assuming the public option stays dead—is an insurance "exchange," through which individuals and families could choose from a menu of standardized policies offered at heavily subsidized rates, provided that their employers do not offer coverage. The subsidies are distributed on a sliding scale based on income, and according to the Congressional Budget Office 23 million people will participate a decade from now, at a cost to taxpayers of some $461 billion.
Think about a family of four earning $42,000 in 2016, which is between 150% and 200% of the federal poverty level. CBO says a mid-level "silver" plan will cost about $14,700 in premiums, of which the family will pay $2,600—since the government would pay the other $12,100. If the family breadwinner (or breadwinners, because the subsidies are based on combined gross income) then gets a raise or works overtime and wages rise to $54,000, the subsidy drops to $9,900. That amounts to an implicit 34% tax on each additional dollar of income.
Or consider a single worker earning $20,600 and buying an individual "silver" policy with a premium at $5,000. Again according to CBO, if his income rises to $26,500, his subsidy plummets to $2,700 from $4,400 (including a cost-sharing subsidy that goes away). This is a 29% marginal tax; moving to other income levels yields increases in the neighborhood of 20% to 23% for both individuals and families. Jim Capretta, a fellow at the Ethics and Public Policy Center, calculates that when combined with other policies like the Earned Income Tax Credit that also phase out, the effective marginal rate would rise to nearly 70% at twice the poverty level.
The incentives for low-wage workers are especially perverse. The exchanges give them a huge break and then take it away gradually as their income goes up. Usually such phase-outs are used to make sure "the rich" don't benefit from IRS dispensations, but here they will have a giant effect on decisions about whether and how much to work, since each additional hour worked reduces the subsidy.
As CBO noted in a July health brief, "Higher [marginal] tax rates also reduce people's incentive to raise their income in other ways, such as working harder in the hope of winning raises; accepting new positions or responsibilities with higher compensation; or investing in their future earning capacity through education, training or other means." This disincentive effect will be especially hard on workers in the middle of their careers and who may not see the same potential for upward mobility as younger workers, but who could earn more through work and effort.
These marginal rate "cliffs" are also a sneaky way for Congress to lower the "scorable" cost of the bill without appearing to do so, because diminishing these rate hikes would boost the total cost of the subsidy. For the same reason, the subsidy is only extended to certain favored people, making it deeply unfair to those not allowed into the exchanges. Families earning identical amounts of money could pay wildly different taxes—a family earning $42,000 and getting insurance through an employer wouldn't receive close to $12,100 from the current tax exclusion for employer-sponsored coverage—while some families earning more money than others will pay significantly lower taxes.
This is an equity catastrophe waiting to happen—and senior Democrats know it. They're laying a political booby-trap that will transfer even more health spending to government after ObamaCare passes.
A far better and cleaner alternative would be to extend the same tax exclusions to individuals that employees receive if they get coverage from their employers. The current bias for one type of insurance has persisted for decades despite its unfairness and irrationality. But ObamaCare will keep all that, while in the process creating many new problems.
__________
The Wall Street Journal published an OpEd on October 20, 2009, titled, "What Singapore can teach the White House, praising the Singapore's health care system, see http://online.wsj.com/article/SB10001424052748704500604574483712417152696.html
The Dutch also appear to have an excellent health system, see http://takingnote.tcf.org/2008/06/the-dutch-healt.html
Middle-income families will face a big marginal rate increase.
None of the new distortions that the Senate health-care bill will layer onto the already-distorted tax code have received the attention they deserve, but in particular its effects on marginal tax rates could use scrutiny. Incredibly, for those with lower incomes, ObamaCare will impose a penalty as high as 34% on . . . work.
Central to Max Baucus's plan—assuming the public option stays dead—is an insurance "exchange," through which individuals and families could choose from a menu of standardized policies offered at heavily subsidized rates, provided that their employers do not offer coverage. The subsidies are distributed on a sliding scale based on income, and according to the Congressional Budget Office 23 million people will participate a decade from now, at a cost to taxpayers of some $461 billion.
Think about a family of four earning $42,000 in 2016, which is between 150% and 200% of the federal poverty level. CBO says a mid-level "silver" plan will cost about $14,700 in premiums, of which the family will pay $2,600—since the government would pay the other $12,100. If the family breadwinner (or breadwinners, because the subsidies are based on combined gross income) then gets a raise or works overtime and wages rise to $54,000, the subsidy drops to $9,900. That amounts to an implicit 34% tax on each additional dollar of income.
Or consider a single worker earning $20,600 and buying an individual "silver" policy with a premium at $5,000. Again according to CBO, if his income rises to $26,500, his subsidy plummets to $2,700 from $4,400 (including a cost-sharing subsidy that goes away). This is a 29% marginal tax; moving to other income levels yields increases in the neighborhood of 20% to 23% for both individuals and families. Jim Capretta, a fellow at the Ethics and Public Policy Center, calculates that when combined with other policies like the Earned Income Tax Credit that also phase out, the effective marginal rate would rise to nearly 70% at twice the poverty level.
The incentives for low-wage workers are especially perverse. The exchanges give them a huge break and then take it away gradually as their income goes up. Usually such phase-outs are used to make sure "the rich" don't benefit from IRS dispensations, but here they will have a giant effect on decisions about whether and how much to work, since each additional hour worked reduces the subsidy.
As CBO noted in a July health brief, "Higher [marginal] tax rates also reduce people's incentive to raise their income in other ways, such as working harder in the hope of winning raises; accepting new positions or responsibilities with higher compensation; or investing in their future earning capacity through education, training or other means." This disincentive effect will be especially hard on workers in the middle of their careers and who may not see the same potential for upward mobility as younger workers, but who could earn more through work and effort.
These marginal rate "cliffs" are also a sneaky way for Congress to lower the "scorable" cost of the bill without appearing to do so, because diminishing these rate hikes would boost the total cost of the subsidy. For the same reason, the subsidy is only extended to certain favored people, making it deeply unfair to those not allowed into the exchanges. Families earning identical amounts of money could pay wildly different taxes—a family earning $42,000 and getting insurance through an employer wouldn't receive close to $12,100 from the current tax exclusion for employer-sponsored coverage—while some families earning more money than others will pay significantly lower taxes.
This is an equity catastrophe waiting to happen—and senior Democrats know it. They're laying a political booby-trap that will transfer even more health spending to government after ObamaCare passes.
A far better and cleaner alternative would be to extend the same tax exclusions to individuals that employees receive if they get coverage from their employers. The current bias for one type of insurance has persisted for decades despite its unfairness and irrationality. But ObamaCare will keep all that, while in the process creating many new problems.
__________
The Wall Street Journal published an OpEd on October 20, 2009, titled, "What Singapore can teach the White House, praising the Singapore's health care system, see http://online.wsj.com/article/SB10001424052748704500604574483712417152696.html
The Dutch also appear to have an excellent health system, see http://takingnote.tcf.org/2008/06/the-dutch-healt.html
Labels:
health plan
Friday, October 16, 2009
Stimulus jobs report 'rife with mistakes'
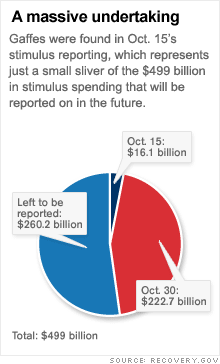
http://money.cnn.com/2009/10/16/news/economy/stimulus_jobs/index.htm
On stimulus jobs reporting, a big 'Oops'
Error in Recovery Act accounting raises doubts about government's ability to precisely track the flow of funds and jobs.
By David Goldman, CNNMoney.com staff writer
Last Updated: October 16, 2009: 4:53 PM ET
NEW YORK (CNNMoney.com) -- Gaffes in federal reports this week about stimulus have called into question the government's ability to accurately track how many jobs are being created by the massive $787 billion Recovery Act.
The data in Thursday's reports were filled with mistakes, including an error that made it look like a French vaccine maker received the largest stimulus contract, $1.4 billion, when in fact it has gotten an award one-100th the size.
Government research organization OMB Watch said its assessment of the reports revealed many inconsistencies in the job data.
"The data is rife with mistakes," said Craig Jennings, senior federal fiscal policy analyst at OMB Watch. "When you put out data that hasn't yet been checked, it undermines transparency, because you are putting out wrong information."
According to the Recovery Board, a non-profit, government-funded organization that operates stimulus data tracker recovery.gov, the government expected mistakes and is reviewing reports of them.
Uncovering how many jobs stimulus created is critical to the debate about the Recovery Act's value. Critics argue that the mammoth funding simply represents more government spending and is not effectively being used to create jobs. But proponents say stimulus is a crucial shot in the arm for the economy, and that the labor market would have fallen further without it.
"Understanding how many jobs are created will answer the very fair and important question, 'What return on our investment are we getting?' " said Christopher Mihm, the Government Accountability Office's managing director of strategic issues.
But the enormity of the stimulus bill leaves some experts saying it will be impossible to accurately portray the data. The sheer size of the reporting is dumbfounding: Tens of thousands of recipients will file reports after receiving stimulus funds from one of 28 government umbrella agencies, or from one of countless agencies from the 50 states.
Making it even more difficult to discover the true jobs number is a decision to put the responsibility of correcting mistakes on the stimulus recipients' shoulders. For transparency's sake, government agencies can point out errors but are powerless to change them. All of the data are under government review, and a report on the errors the agencies find will be available at the end of the month.
"It's important that those errors get caught before they get published, and right now they're still under review," said Jennings. "It's possible that some will be caught by the review, but it will take an incredible amount of man power just to sift through the data."
Recipients of stimulus funds were required to report how many jobs they saved or created and how much money they have received from government agencies by Oct. 10. The first sliver of that information was posted on recovery.gov on Thursday, with much more data to come on Oct. 30.
The contract awards posted Thursday represented less than 7% of the total stimulus funds doled out so far. By far the largest part of stimulus is in grants to states, which account for 83% of stimulus funding. Federal agencies and recipients are spending nearly three weeks reviewing these state reports to improve their accuracy before publishing them.
Loans to recipients make up the other 10%. Both grants and loans will be posted on recovery.gov at the end of the month.
There were 5,232 federal contracts reported Thursday, but 41,944 grants and loans will be reported on Oct. 30. Gov. Arnold Schwarzenegger of California recently said that his state alone submitted 5,747 reports from agencies and others who received funds from the state.
Mistake-prone reporting
A mistake in the very first contract listed on the site prompted doubts about the reliability of the reports.
Recovery.gov erroneously reported Thursday that French vaccine maker Sanofi Pasteur had received $1.4 billion in stimulus funds from the Department of Health and Human Services. The company topped the site's list titled "Largest federal contracts in U.S."
When CNNMoney.com first asked about the contract on Thursday, a spokeswoman from Sanofi Pasteur suspected the $1.4 billion figure was a mistake. HHS spokeswoman Vicki Rivas-Vazquez said the number on recovery.gov was erroneous and the actual amount was $10.4 million.
Sanofi Pasteur said Friday that $10.4 million is the correct figure.
"We anticipated errors in the reporting and so informed many reporters beforehand," said Edward Pound, spokesman for the Recovery Board. "This is the first time this kind of reporting is being done. These reports are being reviewed by federal agencies and recipients to catch any errors or problems."
The Recovery Board has the tall task of compiling all of the data, and is spending $18 million revamping its Web site to manage all of the information.
OMB Watch said its review yielded "really weird job numbers," including many discrepancies within the reports themselves. For instance, Jennings said OMB Watch found that many companies said in a narrative portion of their reports that it was able to retain several employees because of stimulus funds, but the "jobs created" column read "zero."
The Recovery Board aggregates its jobs data from the "jobs created" column to display the total number of jobs saved or created. Jennings speculated that recipients might have been confused about the scope of the term "created."
"I would not stake any sort of claims on those job numbers," said Jennings. "We don't know what's going on there."
Even the job figures that are input correctly do not always reflect the true number of positions created by stimulus funds.
For instance, UT-Battelle received a $338.7 million contract, listed as the fourth largest on the recovery.gov site. So far, the company, which manages Oak Ridge National Laboratory in Tennessee for the Department of Energy, has spent $13 million and created 41 jobs, mostly related to the oversight of subcontractors.
But the funding is actually creating many more jobs, said Thom Mason, UT-Battelle's CEO. Among the firm's first stimulus projects is the building of a chemistry and new materials research lab, which will employ 150 construction workers. None of these positions will appear on UT-Battelle's reports to the federal government.
"It's important that everyone reports on a consistent basis," said Mason, who expects to hire up to 4,000 subcontractors with stimulus funds. "The difficulty is that it gives you a number that's not really a realistic reflection of how many jobs are created."
--CNNMoney.com senior writer Tami Luhby contributed to this report. To top of page
2010 COLA Limits for Employee Plans
The 2010 Cost-of-Living Adjustments (COLAs) for determining annual limits for most retirement plans remain the same as in 2009, except for the following:
- The modified adjusted gross income limits for determining the deductible amount of traditional IRA contributions for single and head of household filers who are active participants in a plan, and for married taxpayers filing jointly who aren’t active participants in a plan but whose spouses are;
- The modified adjusted gross income for Roth IRA purposes for determining the maximum Roth IRA contributions for taxpayers whose filing status is married filing jointly or qualifying widow(er); and
- The adjusted gross income limits for taxpayers who qualify for the 50% savers credit.
Labels:
COLA,
retirement plan
Making Sense of High-Deductible Health Plans
http://www.nytimes.com/2009/10/17/health/17patient.html
By WALECIA KONRAD
Published: October 16, 2009
And now comes the pitch: What can you do to reduce health care costs?
During the open enrollment season for employee benefits, now under way for next year, you are likely to hear a whole lot about Consumer-Directed Health Plans. You, of course, are the consumer. And you’re being directed to save your employer a lot of money — so much so that many employers are offering workers lucrative incentives to make the switch into a consumer-directed plan.
Should you bite? And if you don’t have a choice — General Electric, for example, is forcing 75,000 of its salaried employees in the United States to choose one of three consumer-driven options — how can you best navigate this new landscape? In this column we’ll offer the latest expert advice. But first, some background.
Consumer-directed health plans, in essence, are high-deductible health insurance. The plans charge a high annual deductible — starting at $1,200 for single employees and $2,400 for families in 2010 — in exchange for lower monthly premiums. And in many cases, there is also a tax break.
The idea behind the “consumer directed” part goes like this: If you and I are spending more of our own money on health care, then we are likely to ask doctors and hospitals many more questions upfront and be more careful about which tests and procedures we receive. After all, until we exhaust that high annual deductible, it’s our money on the line.
Employers are pushing these plans because they can save the company as much as 20 percent, compared with traditional insurance. The number of workers enrolled in high-deductible plans at companies with more than 200 employees reached an estimated 22 percent in 2009, from 10 percent in 2006, according to a study of more than 2,000 companies conducted by the Kaiser Family Foundation.
Most corporate high-deductible plans come with a health savings account, which allows employees to deposit tax-free dollars to help offset the higher out-of-pocket costs. A person can sock away up to $3,050 in 2010 in these accounts, $6,150 for a family. Many companies will contribute a lump sum to your account — anywhere from $500 to $1,000 — as an incentive for you to sign up for the plan.
The tax break on these accounts can be considerable, in theory at least: You deposit any contributions pre-tax, and any earnings grow tax-free, and there is no tax when you withdraw funds to pay for eligible health care expenses.
Unlike the lose-it-or-use-it flexible spending accounts, any health savings money you do not use one year rolls over into the next. And because a health savings account is in your name, you take it with you — along with any employer contributions — if you leave the company.
Another common health savings account, especially at smaller companies, is called the Health Reimbursement Arrangement. These accounts can be linked to any type of health insurance policy but are most typically used with high-deductible plans. This account is totally financed by the company. Your employer earmarks a certain amount of money for you to help pay higher health care costs, and it is up to the employer to decide if it will credit any interest earned to your account or if the money will roll over from year to year. In most cases, you cannot take this account with you if you leave that job.
Some employers offer only the high-deductible plan itself. In that case, if the policy meets certain government regulations, you can set up your own health savings account. For more information on how to do that, go to www.treas.gov/offices/public-affairs/hsa/faq_setup.shtml or check with your bank, which will often help you set up an account. Also, check with your human resources department to see if it will set up a direct deposit arrangement for your account.
O.K., so there’s the primer.
What may happen with such insurance offerings in the future, after Washington gets through rethinking the nation’s health care system, is anyone’s guess. But for now, you’ve got to plan what you want your own personal health care system to look like starting in January. So consider these factors before taking the high-deductible plunge:
HIGH-DEDUCTIBLE VS. TRADITIONAL PLANS If your company is still offering both alternatives, here are some questions to ask yourself to help compare the two choices.
What are my health expectations this year? Young, relatively healthy people can benefit from the lower premiums a high-deductible plan offers (usually about 20 percent less than traditional insurance), while still having coverage in a medical crisis.
But if you have a chronic condition like asthma or diabetes, or you know you’re headed for, say, knee surgery come January, you’ll need to sit down and do the math to figure out which plan will cost you more money, says Dean Hatfield, a senior vice president at Sibson Consulting. And here’s a surprise: It won’t always be the high-deductible plan.
That is because many employers are raising premiums on traditional H.M.O. and P.P.O. plans as a way to further encourage employees to pick the high-deductible option. So those higher premiums might come closer to offsetting the higher out-of-pocket costs of the high-deductible plans.
What’s more, high-deductible plans that qualify for a health savings account must meet government regulations limiting the amount you’ll pay out of pocket. For 2010, those limits are $5,950 for individuals and $11,900 for families, including the cost of the deductibles. (Be sure to check the policy’s benefits summary for out-of-pocket maximums.)
How much can I afford to contribute each month? If you don’t have an extra cent to put into some kind of health savings account, the savings from the lower premiums on the high-deductible plan will typically not be enough to compensate for your out-of-pocket costs for any unexpected emergencies. If something drastic happens, you may quickly find yourself in debt. These plans work best for people with enough discretionary income to finance their plans, says Gary Claxton, a vice president at the Kaiser Family Foundation.
Where are my doctors? The high-deductible choice may use a different network of health care providers than the insurance plan you use now. You’ll want to make sure you can still see your doctors and other health care providers.
On the other hand, your employer may be changing the other network options as well. And so you may find your doctors are more accessible through the high-deductible offering than the new P.P.O.’s or H.M.O.’s that you might have to switch to, anyway. The only way to know for sure is to check.
SAVINGS ACCOUNTS VS. REIMBURSEMENT ACCOUNTS In most cases, employees won’t have a choice between these two savings vehicles. Most employers offer one or the other.
But if your company happens to offer both, as General Electric is doing, the decision may boil down to how long you think you’ll be with that employer. If it’s long enough to take advantage of the company-financed reimbursement account for the year’s deductibles, then you may want your employer to pick up the tab. If you know you’re going to make a change soon, though, or you’re worried about your job stability, the portable health savings account with a company contribution and its tax advantages may make more sense.
EMPLOYEE INCENTIVES Beyond contributions to your health savings account, some employers are offering other incentives that may be easy to overlook, Mr. Hatfield said.
For instance, employers in recent years have been pushing workers to fill out health questionnaires and even offering an extra $100 or so in contribution to their health savings accounts if they comply. This year, however, you may receive the bonus only if you and your spouse both fill out the questionnaire, Mr. Hatfield said. Be sure to read all of your enrollment materials carefully, and don’t be afraid to call your benefits department and ask what incentives are available.
Next week, as Patient Money continues to guide you through open-enrollment season, my colleague Lesley Alderman will offer advice for employees who find they are forced to switch health insurance plans.
By WALECIA KONRAD
Published: October 16, 2009
And now comes the pitch: What can you do to reduce health care costs?
During the open enrollment season for employee benefits, now under way for next year, you are likely to hear a whole lot about Consumer-Directed Health Plans. You, of course, are the consumer. And you’re being directed to save your employer a lot of money — so much so that many employers are offering workers lucrative incentives to make the switch into a consumer-directed plan.
Should you bite? And if you don’t have a choice — General Electric, for example, is forcing 75,000 of its salaried employees in the United States to choose one of three consumer-driven options — how can you best navigate this new landscape? In this column we’ll offer the latest expert advice. But first, some background.
Consumer-directed health plans, in essence, are high-deductible health insurance. The plans charge a high annual deductible — starting at $1,200 for single employees and $2,400 for families in 2010 — in exchange for lower monthly premiums. And in many cases, there is also a tax break.
The idea behind the “consumer directed” part goes like this: If you and I are spending more of our own money on health care, then we are likely to ask doctors and hospitals many more questions upfront and be more careful about which tests and procedures we receive. After all, until we exhaust that high annual deductible, it’s our money on the line.
Employers are pushing these plans because they can save the company as much as 20 percent, compared with traditional insurance. The number of workers enrolled in high-deductible plans at companies with more than 200 employees reached an estimated 22 percent in 2009, from 10 percent in 2006, according to a study of more than 2,000 companies conducted by the Kaiser Family Foundation.
Most corporate high-deductible plans come with a health savings account, which allows employees to deposit tax-free dollars to help offset the higher out-of-pocket costs. A person can sock away up to $3,050 in 2010 in these accounts, $6,150 for a family. Many companies will contribute a lump sum to your account — anywhere from $500 to $1,000 — as an incentive for you to sign up for the plan.
The tax break on these accounts can be considerable, in theory at least: You deposit any contributions pre-tax, and any earnings grow tax-free, and there is no tax when you withdraw funds to pay for eligible health care expenses.
Unlike the lose-it-or-use-it flexible spending accounts, any health savings money you do not use one year rolls over into the next. And because a health savings account is in your name, you take it with you — along with any employer contributions — if you leave the company.
Another common health savings account, especially at smaller companies, is called the Health Reimbursement Arrangement. These accounts can be linked to any type of health insurance policy but are most typically used with high-deductible plans. This account is totally financed by the company. Your employer earmarks a certain amount of money for you to help pay higher health care costs, and it is up to the employer to decide if it will credit any interest earned to your account or if the money will roll over from year to year. In most cases, you cannot take this account with you if you leave that job.
Some employers offer only the high-deductible plan itself. In that case, if the policy meets certain government regulations, you can set up your own health savings account. For more information on how to do that, go to www.treas.gov/offices/public-affairs/hsa/faq_setup.shtml or check with your bank, which will often help you set up an account. Also, check with your human resources department to see if it will set up a direct deposit arrangement for your account.
O.K., so there’s the primer.
What may happen with such insurance offerings in the future, after Washington gets through rethinking the nation’s health care system, is anyone’s guess. But for now, you’ve got to plan what you want your own personal health care system to look like starting in January. So consider these factors before taking the high-deductible plunge:
HIGH-DEDUCTIBLE VS. TRADITIONAL PLANS If your company is still offering both alternatives, here are some questions to ask yourself to help compare the two choices.
What are my health expectations this year? Young, relatively healthy people can benefit from the lower premiums a high-deductible plan offers (usually about 20 percent less than traditional insurance), while still having coverage in a medical crisis.
But if you have a chronic condition like asthma or diabetes, or you know you’re headed for, say, knee surgery come January, you’ll need to sit down and do the math to figure out which plan will cost you more money, says Dean Hatfield, a senior vice president at Sibson Consulting. And here’s a surprise: It won’t always be the high-deductible plan.
That is because many employers are raising premiums on traditional H.M.O. and P.P.O. plans as a way to further encourage employees to pick the high-deductible option. So those higher premiums might come closer to offsetting the higher out-of-pocket costs of the high-deductible plans.
What’s more, high-deductible plans that qualify for a health savings account must meet government regulations limiting the amount you’ll pay out of pocket. For 2010, those limits are $5,950 for individuals and $11,900 for families, including the cost of the deductibles. (Be sure to check the policy’s benefits summary for out-of-pocket maximums.)
How much can I afford to contribute each month? If you don’t have an extra cent to put into some kind of health savings account, the savings from the lower premiums on the high-deductible plan will typically not be enough to compensate for your out-of-pocket costs for any unexpected emergencies. If something drastic happens, you may quickly find yourself in debt. These plans work best for people with enough discretionary income to finance their plans, says Gary Claxton, a vice president at the Kaiser Family Foundation.
Where are my doctors? The high-deductible choice may use a different network of health care providers than the insurance plan you use now. You’ll want to make sure you can still see your doctors and other health care providers.
On the other hand, your employer may be changing the other network options as well. And so you may find your doctors are more accessible through the high-deductible offering than the new P.P.O.’s or H.M.O.’s that you might have to switch to, anyway. The only way to know for sure is to check.
SAVINGS ACCOUNTS VS. REIMBURSEMENT ACCOUNTS In most cases, employees won’t have a choice between these two savings vehicles. Most employers offer one or the other.
But if your company happens to offer both, as General Electric is doing, the decision may boil down to how long you think you’ll be with that employer. If it’s long enough to take advantage of the company-financed reimbursement account for the year’s deductibles, then you may want your employer to pick up the tab. If you know you’re going to make a change soon, though, or you’re worried about your job stability, the portable health savings account with a company contribution and its tax advantages may make more sense.
EMPLOYEE INCENTIVES Beyond contributions to your health savings account, some employers are offering other incentives that may be easy to overlook, Mr. Hatfield said.
For instance, employers in recent years have been pushing workers to fill out health questionnaires and even offering an extra $100 or so in contribution to their health savings accounts if they comply. This year, however, you may receive the bonus only if you and your spouse both fill out the questionnaire, Mr. Hatfield said. Be sure to read all of your enrollment materials carefully, and don’t be afraid to call your benefits department and ask what incentives are available.
Next week, as Patient Money continues to guide you through open-enrollment season, my colleague Lesley Alderman will offer advice for employees who find they are forced to switch health insurance plans.
Labels:
health plan
Thursday, October 15, 2009
No 2010 increase in Social Security
http://money.cnn.com/2009/10/14/news/economy/obama_seniors_payment/index.htm
Seniors' benefits will not be adjusted for cost of living because of low consumer prices. Obama urges $250 emergency payments.
By Jeanne Sahadi, CNNMoney.com senior writer
Last Updated: October 15, 2009: 9:55 AM ET
NEW YORK (CNNMoney.com) -- There will be no cost-of-living increase for 57 million Social Security beneficiaries next year because consumer prices have fallen, the Social Security Administration announced on Thursday.
It marks the first time that Social Security benefits have not been increased year over year since the cost-of-living adjustment was put into effect in 1975.
To help counterbalance the hit, President Obama is calling on Congress to send another $250 relief payment to seniors and other Americans to stem the economic strain.
"Even as we seek to bring about recovery, we must act on behalf of those hardest hit by this recession," Obama said in a statement Wednesday. "That is why I am announcing my support for an additional $250 in emergency recovery assistance to seniors, veterans, and people with disabilities to help them make it through these difficult times."
Last year, Social Security beneficiaries got a 5.8% cost-of-living adjustment, the largest since 1982, largely because of the spike in energy prices.
"This year, in light of the human need, we need to support President Obama's call for us to make another $250 recovery payment for 57 million Americans," said Commissioner of Social Security Michael J. Astrue in a written statement.
Since there will be no COLA for benefits, the law also prohibits the Social Security Administration from increasing the maximum amount of earnings subject to the Social Security tax. This year and next, the first $106,800 of a worker's earnings is subject to the 12.4% Social Security tax. Workers typically pay half of that and their employer pay the other half.
It's still not clear yet what if any changes will be made to seniors' Medicare Part B premiums for hospital care next year. The Social Security Administration said in its announcement that if there is an increase that a "hold harmless" provision in the law would protect 93% of Social Security beneficiaries from the increase.
New emergency payment similar to COLA
Obama's proposed $250 payment is roughly equal to a 2% increase in benefits for the average Social Security beneficiary.
Congress approved a similar payment as part of the $787 billion economic recovery act enacted in February.
As with the first $250 recovery payment, the second one would be exempt from income tax, a senior administration official said in a call with reporters on Wednesday.
If approved by Congress, the payments would be sent out in 2010, most likely in the first half. "It wouldn't be late in 2010," the administration official said.
The measure would cost $13 billion over 10 years, according to White House estimates.
The call for increased benefits for seniors is one of several proposals to expand stimulus benefits. Lawmakers are also considering extending unemployment benefits and the homebuyer tax credit, both of which were included in the economic stimulus bill passed in February.
In addition to the $250 emergency payments, the White House has also publicly supported the extension of jobless benefits as well as the extension of subsidies to help the unemployed purchase health insurance under Cobra. The president has not said yet whether he supports the expansion of the homebuyer tax credit.
First Published: October 14, 2009: 5:00 PM ET
Seniors' benefits will not be adjusted for cost of living because of low consumer prices. Obama urges $250 emergency payments.
By Jeanne Sahadi, CNNMoney.com senior writer
Last Updated: October 15, 2009: 9:55 AM ET
NEW YORK (CNNMoney.com) -- There will be no cost-of-living increase for 57 million Social Security beneficiaries next year because consumer prices have fallen, the Social Security Administration announced on Thursday.
It marks the first time that Social Security benefits have not been increased year over year since the cost-of-living adjustment was put into effect in 1975.
To help counterbalance the hit, President Obama is calling on Congress to send another $250 relief payment to seniors and other Americans to stem the economic strain.
"Even as we seek to bring about recovery, we must act on behalf of those hardest hit by this recession," Obama said in a statement Wednesday. "That is why I am announcing my support for an additional $250 in emergency recovery assistance to seniors, veterans, and people with disabilities to help them make it through these difficult times."
Last year, Social Security beneficiaries got a 5.8% cost-of-living adjustment, the largest since 1982, largely because of the spike in energy prices.
"This year, in light of the human need, we need to support President Obama's call for us to make another $250 recovery payment for 57 million Americans," said Commissioner of Social Security Michael J. Astrue in a written statement.
Since there will be no COLA for benefits, the law also prohibits the Social Security Administration from increasing the maximum amount of earnings subject to the Social Security tax. This year and next, the first $106,800 of a worker's earnings is subject to the 12.4% Social Security tax. Workers typically pay half of that and their employer pay the other half.
It's still not clear yet what if any changes will be made to seniors' Medicare Part B premiums for hospital care next year. The Social Security Administration said in its announcement that if there is an increase that a "hold harmless" provision in the law would protect 93% of Social Security beneficiaries from the increase.
New emergency payment similar to COLA
Obama's proposed $250 payment is roughly equal to a 2% increase in benefits for the average Social Security beneficiary.
Congress approved a similar payment as part of the $787 billion economic recovery act enacted in February.
As with the first $250 recovery payment, the second one would be exempt from income tax, a senior administration official said in a call with reporters on Wednesday.
If approved by Congress, the payments would be sent out in 2010, most likely in the first half. "It wouldn't be late in 2010," the administration official said.
The measure would cost $13 billion over 10 years, according to White House estimates.
The call for increased benefits for seniors is one of several proposals to expand stimulus benefits. Lawmakers are also considering extending unemployment benefits and the homebuyer tax credit, both of which were included in the economic stimulus bill passed in February.
In addition to the $250 emergency payments, the White House has also publicly supported the extension of jobless benefits as well as the extension of subsidies to help the unemployed purchase health insurance under Cobra. The president has not said yet whether he supports the expansion of the homebuyer tax credit.
First Published: October 14, 2009: 5:00 PM ET
Labels:
Social Security
Foreclosures rise 5 percent from summer to fall
http://news.yahoo.com/s/ap/20091015/ap_on_bi_ge/us_foreclosure_rates
By ALAN ZIBEL, AP Real Estate Writer Alan Zibel, Ap Real Estate Writer – Thu Oct 15, 5:12 am ET
WASHINGTON – The number of households caught up in the foreclosure crisis rose more than 5 percent from summer to fall as a federal effort to assist struggling borrowers was overwhelmed by a flood of defaults among people who lost their jobs.
The foreclosure crisis affected nearly 938,000 properties in the July-September quarter, compared with about 890,000 in the prior three months, according to a report released Thursday by RealtyTrac Inc. That puts foreclosure-related filings on a pace to hit about 3.5 million this year, up from more than 2.3 million last year.
Unemployment is the main reason homeowners are falling into trouble. While the economy is likely out of recession, the unemployment rate — now at a 26-year high of 9.8 percent — isn't expected to peak until the middle of next year.
Mortgage companies sometimes allow unemployed homeowners to defer three to six months of payments while they are looking for a job. But there's little else they can do.
"The sheer scale of the problem is preventing the loan modification programs from having the kind of impact we'd all like" said Rick Sharga, RealtyTrac's senior vice president for marketing.
Last week, the Obama administration hailed a milestone in its mortgage relief effort, reporting that 500,000 homeowners have received help since the program was launched in March. But new defaults are still exceeding the number of borrowers getting help.
Mortgage companies have slowed down the pace of foreclosures as they evaluate whether borrowers qualify for the administration's program. Analysts, however, forecast that many of those homeowners won't qualify, and foresee a new wave of foreclosed properties hitting the market next year. That's likely to further depress home prices.
Some homeowners are in such a massive financial hole that it's hard to design a modification that will actually provide lower payments. And some have avoided paying their monthly bills for a long time.
Carlos Estrada, 57, of Tulare, Calif., for example, hasn't made a mortgage payment since February 2008. The construction jobs that kept him working more than 40 hours a week during the housing boom have all but vanished.
Earlier this year, he turned down a modification offer from Bank of America because it would have incorporated his unpaid balance and raised his monthly bill. But a bank spokeswoman said Wednesday that Estrada's foreclosure sale had been postponed until late next month while the bank reviews whether he can qualify for help.
"I'm still here waiting for them to help me resolve this situation," Estrada said in Spanish.
According to the RealtyTrac report, there were nearly 344,000 foreclosure-related filings last month, down 4 percent from a month earlier but still the third-highest month since the report started in early 2005.
It was the seventh-straight month in which more than 300,000 households receiving a foreclosure filing, which includes default notices and several other legal notices that homeowners receive before they finally lose their homes.
Banks repossessed nearly 88,000 homes in September, up from about 76,000 a month earlier.
On a state-by-state basis, Nevada had the nation's highest foreclosure rate in the July-September quarter. Arizona was No. 2, followed by California, Florida and Idaho. Rounding out the top 10 were Utah, Georgia, Michigan, Colorado and Illinois.
__
AP Real Estate Writer Alex Veiga contributed to this report from Los Angeles.
By ALAN ZIBEL, AP Real Estate Writer Alan Zibel, Ap Real Estate Writer – Thu Oct 15, 5:12 am ET
WASHINGTON – The number of households caught up in the foreclosure crisis rose more than 5 percent from summer to fall as a federal effort to assist struggling borrowers was overwhelmed by a flood of defaults among people who lost their jobs.
The foreclosure crisis affected nearly 938,000 properties in the July-September quarter, compared with about 890,000 in the prior three months, according to a report released Thursday by RealtyTrac Inc. That puts foreclosure-related filings on a pace to hit about 3.5 million this year, up from more than 2.3 million last year.
Unemployment is the main reason homeowners are falling into trouble. While the economy is likely out of recession, the unemployment rate — now at a 26-year high of 9.8 percent — isn't expected to peak until the middle of next year.
Mortgage companies sometimes allow unemployed homeowners to defer three to six months of payments while they are looking for a job. But there's little else they can do.
"The sheer scale of the problem is preventing the loan modification programs from having the kind of impact we'd all like" said Rick Sharga, RealtyTrac's senior vice president for marketing.
Last week, the Obama administration hailed a milestone in its mortgage relief effort, reporting that 500,000 homeowners have received help since the program was launched in March. But new defaults are still exceeding the number of borrowers getting help.
Mortgage companies have slowed down the pace of foreclosures as they evaluate whether borrowers qualify for the administration's program. Analysts, however, forecast that many of those homeowners won't qualify, and foresee a new wave of foreclosed properties hitting the market next year. That's likely to further depress home prices.
Some homeowners are in such a massive financial hole that it's hard to design a modification that will actually provide lower payments. And some have avoided paying their monthly bills for a long time.
Carlos Estrada, 57, of Tulare, Calif., for example, hasn't made a mortgage payment since February 2008. The construction jobs that kept him working more than 40 hours a week during the housing boom have all but vanished.
Earlier this year, he turned down a modification offer from Bank of America because it would have incorporated his unpaid balance and raised his monthly bill. But a bank spokeswoman said Wednesday that Estrada's foreclosure sale had been postponed until late next month while the bank reviews whether he can qualify for help.
"I'm still here waiting for them to help me resolve this situation," Estrada said in Spanish.
According to the RealtyTrac report, there were nearly 344,000 foreclosure-related filings last month, down 4 percent from a month earlier but still the third-highest month since the report started in early 2005.
It was the seventh-straight month in which more than 300,000 households receiving a foreclosure filing, which includes default notices and several other legal notices that homeowners receive before they finally lose their homes.
Banks repossessed nearly 88,000 homes in September, up from about 76,000 a month earlier.
On a state-by-state basis, Nevada had the nation's highest foreclosure rate in the July-September quarter. Arizona was No. 2, followed by California, Florida and Idaho. Rounding out the top 10 were Utah, Georgia, Michigan, Colorado and Illinois.
__
AP Real Estate Writer Alex Veiga contributed to this report from Los Angeles.
Labels:
foreclosure
Wednesday, October 14, 2009
Health Insurers Emerge as Obama's Top Foe in Reform Effort
http://www.washingtonpost.com/wp-dyn/content/article/2009/10/13/AR2009101303472.html
By Ceci Connolly
Washington Post Staff Writer
Wednesday, October 14, 2009
Now they have an enemy.
For months, President Obama and his administration waged their fight for a health-care overhaul without a clear opponent, even courting the industry executives and interest groups that helped kill reform efforts 15 years ago.
But attacks on the leading Democratic reform plan this week by the insurance lobby left little doubt that two of the most powerful institutions involved in the debate -- the White House and the nation's insurance companies -- have abandoned any real hope of forging a compromise. What was a tenuous truce has turned quickly into an all-out battle, with both sides ratcheting up the hostilities.
As the Senate Finance Committee on Tuesday approved a 10-year, $829 billion bill to remake the health-care system, Obama's top advisers and the insurers moved into a more intense stage of conflict.
"The insurance industry has decided to lead the charge against health reform, and everyone recognizes their motives: profits," said White House deputy communications director Dan Pfeiffer. "We are going to make sure they can't sink this effort at the last minute."
Pfeiffer castigated the industry for releasing a report Monday that concluded that the finance panel's bill would increase costs for consumers. "They made themselves a very good foil," he said.
The insurers, however, showed no sign of being chastened. America's Health Insurance Plans, an industry trade group, opened a fresh line of attack with a multistate advertising campaign warning that senior citizens enrolled in private Medicare plans could lose benefits under the legislation.
"Is it right to ask 10 million seniors on Medicare Advantage for more than their fair share?" the television spot asks. "Congress is proposing $100 billion in cuts to Medicare Advantage. The nonpartisan Congressional Budget Office says many seniors will see cuts in benefits."
The Finance Committee's bill would reduce spending on the plans AHIP cites by $113 billion over the next decade, which could mean reduced insurer profits, higher co-payments by beneficiaries or fewer extra benefits such as eyeglasses and gym memberships.
"We want to begin to build an awareness of the potential implications to seniors," said AHIP President Karen Ignagni.
She declined to say how much money would be spent on the commercials airing in six states, but one advertising analyst said the industry has enough cash to pose a serious threat. "They can spend whatever they feel they need to influence this," said Evan Tracey, president of the Campaign Media Analysis Group. "Seniors are a very important group politically."
The insurance sector and health maintenance organizations spent more than $116 million on lobbying in the first six months of this year, according to an analysis by the nonpartisan Center for Responsive Politics.
"It's pretty clear now, they intend at the eleventh hour to launch a very expensive and misleading campaign against reform," Pfeiffer said.
From the earliest days of his presidency, Obama approached the health-care debate determined to not repeat the mistakes of President Bill Clinton. Obama invited business leaders to the White House for brainstorming sessions and negotiated deals with several industries, including hospitals and drugmakers. The insurance industry had a seat at the table.
"We had no public face of opposition," Pfeiffer said. Yet all the while, the insurers were "milling around in the background," unable to reach an accord but muted in their objections, he said.
Since Labor Day, the industry has been on the receiving end of more than $25 million in critical advertising, Tracey estimated.
Ignagni complained of a "major effort to discredit and silence" the industry and its allies. "That's just wrong in a democracy."
She stood by the report her group commissioned and said she expects other analyses to reach similar conclusions that the bills now before Congress would not constrain rising medical bills.
As the report has come under fire, PricewaterhouseCoopers has distanced itself somewhat from it. The firm said Monday that AHIP had instructed it to focus on only some features of the bill, while not taking into account other major features such as the effect of subsidies for those buying insurance.
"America's Health Insurance Plans engaged PricewaterhouseCoopers to prepare a report that focused on four components of the Senate Finance Committee proposal," the company said in a statement. "As the report itself acknowledges, other provisions that are part of health reform proposals were not included in the PwC analysis."
Lawmakers were divided on the issue, largely along party lines, with many Democrats suggesting that the industry actions will serve only to further aggravate many voters.
"The insurance industry ought to be ashamed of this report," Sen. John F. Kerry (D-Mass.) said during committee debate.
Sen. Robert Menendez (D-N.J.) said the last-minute attacks by the industry "are one more indicator we're on the right track."
Harvard University pollster Robert Blendon said public opinion remains mixed.
"Most people are afraid these bills are going to raise their costs, so this could raise public anxiety," he said. "At the same time, the health insurance industry is at the bottom of the scale of people's trust."
Sen. Joseph I. Lieberman (I-Conn.) said Tuesday that he would not support the finance panel's bill because of cost concerns.
"I'm afraid that in the end the Baucus bill is actually going to raise the price of insurance for most of the people in the country," he said on Fox Business Network's "Imus in the Morning" program, referring to Finance Chairman Max Baucus (D-Mont.).
In committee debate, Republicans pressed CBO chief Douglas W. Elmendorf on the impact of the bill on total health spending nationwide and on insurance premiums, but he did not take a side in the debate.
"We can't assess the effects on national health expenditures," he said. "There are so many conflicting forces we have not been able to assess the effect on premiums."
Staff writers Dan Eggen and Alec MacGillis contributed to this report
__________
According to USA Today, a coalition of labor unions...will run a series of newspaper advertisements starting today announcing their opposition to the finance bill, said Gregory King, a spokesman with the American Federation of State, County and Municipal Employees. Unions oppose a plan to pay for the bill in part with a 40% tax on high-priced insurance plans.
To read the USA Today article, click on http://www.usatoday.com/news/washington/2009-10-12-healthcare_N.htm
By Ceci Connolly
Washington Post Staff Writer
Wednesday, October 14, 2009
Now they have an enemy.
For months, President Obama and his administration waged their fight for a health-care overhaul without a clear opponent, even courting the industry executives and interest groups that helped kill reform efforts 15 years ago.
But attacks on the leading Democratic reform plan this week by the insurance lobby left little doubt that two of the most powerful institutions involved in the debate -- the White House and the nation's insurance companies -- have abandoned any real hope of forging a compromise. What was a tenuous truce has turned quickly into an all-out battle, with both sides ratcheting up the hostilities.
As the Senate Finance Committee on Tuesday approved a 10-year, $829 billion bill to remake the health-care system, Obama's top advisers and the insurers moved into a more intense stage of conflict.
"The insurance industry has decided to lead the charge against health reform, and everyone recognizes their motives: profits," said White House deputy communications director Dan Pfeiffer. "We are going to make sure they can't sink this effort at the last minute."
Pfeiffer castigated the industry for releasing a report Monday that concluded that the finance panel's bill would increase costs for consumers. "They made themselves a very good foil," he said.
The insurers, however, showed no sign of being chastened. America's Health Insurance Plans, an industry trade group, opened a fresh line of attack with a multistate advertising campaign warning that senior citizens enrolled in private Medicare plans could lose benefits under the legislation.
"Is it right to ask 10 million seniors on Medicare Advantage for more than their fair share?" the television spot asks. "Congress is proposing $100 billion in cuts to Medicare Advantage. The nonpartisan Congressional Budget Office says many seniors will see cuts in benefits."
The Finance Committee's bill would reduce spending on the plans AHIP cites by $113 billion over the next decade, which could mean reduced insurer profits, higher co-payments by beneficiaries or fewer extra benefits such as eyeglasses and gym memberships.
"We want to begin to build an awareness of the potential implications to seniors," said AHIP President Karen Ignagni.
She declined to say how much money would be spent on the commercials airing in six states, but one advertising analyst said the industry has enough cash to pose a serious threat. "They can spend whatever they feel they need to influence this," said Evan Tracey, president of the Campaign Media Analysis Group. "Seniors are a very important group politically."
The insurance sector and health maintenance organizations spent more than $116 million on lobbying in the first six months of this year, according to an analysis by the nonpartisan Center for Responsive Politics.
"It's pretty clear now, they intend at the eleventh hour to launch a very expensive and misleading campaign against reform," Pfeiffer said.
From the earliest days of his presidency, Obama approached the health-care debate determined to not repeat the mistakes of President Bill Clinton. Obama invited business leaders to the White House for brainstorming sessions and negotiated deals with several industries, including hospitals and drugmakers. The insurance industry had a seat at the table.
"We had no public face of opposition," Pfeiffer said. Yet all the while, the insurers were "milling around in the background," unable to reach an accord but muted in their objections, he said.
Since Labor Day, the industry has been on the receiving end of more than $25 million in critical advertising, Tracey estimated.
Ignagni complained of a "major effort to discredit and silence" the industry and its allies. "That's just wrong in a democracy."
She stood by the report her group commissioned and said she expects other analyses to reach similar conclusions that the bills now before Congress would not constrain rising medical bills.
As the report has come under fire, PricewaterhouseCoopers has distanced itself somewhat from it. The firm said Monday that AHIP had instructed it to focus on only some features of the bill, while not taking into account other major features such as the effect of subsidies for those buying insurance.
"America's Health Insurance Plans engaged PricewaterhouseCoopers to prepare a report that focused on four components of the Senate Finance Committee proposal," the company said in a statement. "As the report itself acknowledges, other provisions that are part of health reform proposals were not included in the PwC analysis."
Lawmakers were divided on the issue, largely along party lines, with many Democrats suggesting that the industry actions will serve only to further aggravate many voters.
"The insurance industry ought to be ashamed of this report," Sen. John F. Kerry (D-Mass.) said during committee debate.
Sen. Robert Menendez (D-N.J.) said the last-minute attacks by the industry "are one more indicator we're on the right track."
Harvard University pollster Robert Blendon said public opinion remains mixed.
"Most people are afraid these bills are going to raise their costs, so this could raise public anxiety," he said. "At the same time, the health insurance industry is at the bottom of the scale of people's trust."
Sen. Joseph I. Lieberman (I-Conn.) said Tuesday that he would not support the finance panel's bill because of cost concerns.
"I'm afraid that in the end the Baucus bill is actually going to raise the price of insurance for most of the people in the country," he said on Fox Business Network's "Imus in the Morning" program, referring to Finance Chairman Max Baucus (D-Mont.).
In committee debate, Republicans pressed CBO chief Douglas W. Elmendorf on the impact of the bill on total health spending nationwide and on insurance premiums, but he did not take a side in the debate.
"We can't assess the effects on national health expenditures," he said. "There are so many conflicting forces we have not been able to assess the effect on premiums."
Staff writers Dan Eggen and Alec MacGillis contributed to this report
__________
According to USA Today, a coalition of labor unions...will run a series of newspaper advertisements starting today announcing their opposition to the finance bill, said Gregory King, a spokesman with the American Federation of State, County and Municipal Employees. Unions oppose a plan to pay for the bill in part with a 40% tax on high-priced insurance plans.
To read the USA Today article, click on http://www.usatoday.com/news/washington/2009-10-12-healthcare_N.htm
Labels:
health plan
Senate Finance Committee Passes Health Reform Bill
http://www.webcpa.com/news/Senate-Finance-Committee-Passes-Health-Reform-Bill-52027-1.html
By WebCPA Staff
The Senate Finance Committee has approved its long-awaited version of the health care reform bill by a 14-9 vote.
The lone Republican who voted for the $829 billion bill was Sen. Olympia Snowe of Maine, who joined the 13 Democrats on the committee to pass the measure. Snowe had been intensely involved in the negotiations on the bill as one of the so-called Gang of Six, but her support had been in doubt until the afternoon of the vote. “Is this bill all that I would want?” she said in announcing her support. “Far from it. Is it all that it can be? No. But when history calls, history calls. And I happen to think that the consequences of inaction dictate the urgency of Congress to take every opportunity to demonstrate its capacity to solve the monumental issues of our time.”
The bill will still need to be reconciled with one passed this summer by the Senate Health, Education, Labor & Pensions Committee before it is voted on by the full Senate. The Senate HELP Committee bill contains a number of differences, including a public option run by the government as opposed to the nonprofit health insurance cooperatives in the Finance Committee plan. There are also various tax differences in the Senate Finance Committee bill, including taxes on so-called high-cost “Cadillac” insurance policies. The Finance Committee version of the bill is expected to attract the widest support, however. “Ours is a balanced plan that can pass the Senate,” said Chairman Max Baucus, D-Mont., who shepherded the bill through months of contentious negotiations.
However, ranking member Charles Grassley, R-Iowa, warned, “This bill is already moving on a slippery slope toward more and more government control of health care.” The bill includes a provision that bans insurance companies from denying coverage based on pre-existing conditions, a provision that Republicans had agreed to include. "There's a lot in this bill that's just a consensus that needs to be done, but there are other provisions of this bill that raise a lot of questions," said Grassley.
President Obama, who pushed the committee to complete its work on the bill, praised its passage. “I just want to thank the Senate Finance Committee for plowing forward on what we all acknowledge is an extraordinarily complicated issue,” he said.
Snowe indicated that her vote in the committee was no guarantee of how she would vote on the final bill that comes before the full Senate. “There are many miles to go in this legislative journey,” she said. “My vote is my vote today. It doesn’t forecast what my vote will be tomorrow.”
The bill received some extra support last week when the Congressional Budget Office estimated it would reduce the federal budget by $81 billion over the next decade. However, an insurance industry-sponsored study by PricewaterhouseCoopers released over the weekend threw fresh doubts on the plan, estimating that a family health insurance policy that costs $12,300 today would increase to an average of $25,900 by 2019 if the bill were passed, as opposed to $21,900 under current law.
The study blamed the weakness of the individual mandate requirements and the extra fees imposed on insurance companies for the hike.
Under the bill, a 40 percent excise tax would be imposed on insurers of employer-sponsored plans whose benefits were greater than $8,000 for individuals and $21,000 for families. Annual fees of about $13 billion would be imposed on health insurance companies, pharmaceutical companies and medical device-makers. The threshold for itemized deductions for unreimbursed medical expenses would increase from 7.5 to 10 percent under the bill.
__________
For a full text of the Senate Finance health care bill, click on http://www.opencongress.org/baucus_bill_health_care.html
For a comparison of the Senate Finance Committee bill and the Teddy Kennedy's HELP Committee bill, click on http://www.usatoday.com/news/washington/2009-10-12-healthcare_N.htm#table
By WebCPA Staff
The Senate Finance Committee has approved its long-awaited version of the health care reform bill by a 14-9 vote.
The lone Republican who voted for the $829 billion bill was Sen. Olympia Snowe of Maine, who joined the 13 Democrats on the committee to pass the measure. Snowe had been intensely involved in the negotiations on the bill as one of the so-called Gang of Six, but her support had been in doubt until the afternoon of the vote. “Is this bill all that I would want?” she said in announcing her support. “Far from it. Is it all that it can be? No. But when history calls, history calls. And I happen to think that the consequences of inaction dictate the urgency of Congress to take every opportunity to demonstrate its capacity to solve the monumental issues of our time.”
The bill will still need to be reconciled with one passed this summer by the Senate Health, Education, Labor & Pensions Committee before it is voted on by the full Senate. The Senate HELP Committee bill contains a number of differences, including a public option run by the government as opposed to the nonprofit health insurance cooperatives in the Finance Committee plan. There are also various tax differences in the Senate Finance Committee bill, including taxes on so-called high-cost “Cadillac” insurance policies. The Finance Committee version of the bill is expected to attract the widest support, however. “Ours is a balanced plan that can pass the Senate,” said Chairman Max Baucus, D-Mont., who shepherded the bill through months of contentious negotiations.
However, ranking member Charles Grassley, R-Iowa, warned, “This bill is already moving on a slippery slope toward more and more government control of health care.” The bill includes a provision that bans insurance companies from denying coverage based on pre-existing conditions, a provision that Republicans had agreed to include. "There's a lot in this bill that's just a consensus that needs to be done, but there are other provisions of this bill that raise a lot of questions," said Grassley.
President Obama, who pushed the committee to complete its work on the bill, praised its passage. “I just want to thank the Senate Finance Committee for plowing forward on what we all acknowledge is an extraordinarily complicated issue,” he said.
Snowe indicated that her vote in the committee was no guarantee of how she would vote on the final bill that comes before the full Senate. “There are many miles to go in this legislative journey,” she said. “My vote is my vote today. It doesn’t forecast what my vote will be tomorrow.”
The bill received some extra support last week when the Congressional Budget Office estimated it would reduce the federal budget by $81 billion over the next decade. However, an insurance industry-sponsored study by PricewaterhouseCoopers released over the weekend threw fresh doubts on the plan, estimating that a family health insurance policy that costs $12,300 today would increase to an average of $25,900 by 2019 if the bill were passed, as opposed to $21,900 under current law.
The study blamed the weakness of the individual mandate requirements and the extra fees imposed on insurance companies for the hike.
Under the bill, a 40 percent excise tax would be imposed on insurers of employer-sponsored plans whose benefits were greater than $8,000 for individuals and $21,000 for families. Annual fees of about $13 billion would be imposed on health insurance companies, pharmaceutical companies and medical device-makers. The threshold for itemized deductions for unreimbursed medical expenses would increase from 7.5 to 10 percent under the bill.
__________
For a full text of the Senate Finance health care bill, click on http://www.opencongress.org/baucus_bill_health_care.html
For a comparison of the Senate Finance Committee bill and the Teddy Kennedy's HELP Committee bill, click on http://www.usatoday.com/news/washington/2009-10-12-healthcare_N.htm#table
Labels:
health plan
Tuesday, October 13, 2009
Insurance Dispute Heats Up Before Vote
It does makes sense that lowering the penalty for not buying health insurance from $3,800 to $1,500 per year would reduce the number of healthy people buying insurance as:
Here is a link to the PriceWaterhouseCoopers' report, http://graphics8.nytimes.com/packages/flash/health/pdf/pwc_report_on_Costs_final_101109.pdf
http://www.washingtonpost.com/wp-dyn/content/article/2009/10/12/AR2009101203108.html
Industry Group, White House Spar Over Premiums
By Ceci Connolly
Washington Post Staff Writer
Tuesday, October 13, 2009
Tensions between the White House and insurers exploded into open warfare Monday, with the two sides arguing over what the financial impact of comprehensive health-care legislation moving through Congress would be for average Americans.
As the Senate Finance Committee prepared to vote Tuesday on a 10-year, $829 billion bill, the insurance lobby warned that under the legislation insurance premiums could rise faster and higher than projected.
The Obama administration said the industry analysis was deeply flawed, and its allies lambasted the industry for hypocrisy and an "11th-hour attack" intended to rob President Obama of a victory on his top domestic priority.
"Health insurance companies have been laughing all the way to the bank for generations while people suffer," said Sen. John D. Rockefeller IV (D-W.Va.) "The industry stands today as the greatest impediment to real health-care reform."
The back-and-forth was reminiscent of the health-care debate of 1994, when insurers and other industry leaders helped defeat a similar effort by President Bill Clinton. On Monday, Obama advisers resurrected a report projecting similar premium increases that the industry lobby issued at the height of the Clinton-era debate to argue that the latest analysis is more of the "same old, same old" attacks.
Until now, Obama had succeeded in keeping most of the major interest groups at the bargaining table with the lure of up to 50 million new customers. But insurers have grown increasingly critical of the Finance bill, saying it does not do enough to bring healthy young people into insurance risk pools.
Although the bill would require every American to carry insurance, the committee approved changes that would postpone and reduce penalties on people who do not meet the requirement. The insurance lobby, armed with an analysis by PricewaterhouseCoopers, said that as a result, older, less-healthy patients would be more likely to buy insurance and drive up total costs.
White House budget chief Peter Orszag, citing estimates by the Congressional Budget Office, said that a new insurance marketplace, dubbed an exchange, could attract 22 million customers by 2015.
"It's hard to see how that doesn't provide adequate risk pooling and scaling," he said in an interview Monday.
Nancy-Ann DeParle, director of the White House Office of Health Reform, said the industry study overlooked other provisions of the bill that should ease premium increases. She said tax credits for small businesses and working-class families would help make insurance affordable.
Provisions that allow people to keep the insurance they have and a lower-priced plan for "young invincibles" should also hold down costs, she said.
Karen Ignagni, head of America's Health Insurance Plans, the trade group that released the report, stood by its findings. The CBO estimated that the Finance bill would cover 94 percent of legal residents by 2019, but Ignagni said insurers prefer coverage levels in the "high 90s."
PricewaterhouseCoopers predicted that new industry fees, reductions in Medicare growth and taxes on high-priced "Cadillac" policies would be costs passed on to consumers.
Orszag disputed that notion, arguing that the market will respond to those pressures by developing more affordable products.
"Almost every economist believes the effect of the Cadillac provision would be to reduce premiums over time by leading to more efficient insurance plans," he said.
Over time, a reduction in health-care spending should lead to higher wages, Orszag added.
As analysts debated the long-term effects of legislation that would restructure one-sixth of the economy, Obama's political supporters moved quickly to discredit the insurers.
Ron Pollack, executive director of the pro-reform group Families USA, said the industry report "gives hypocrisy a bad name. . . . They are like a poker player who complains about his hand when, in fact, he is the dealer."
__________
More on the dispute at:
http://www.politico.com/news/stories/1009/28213.html#
http://prescriptions.blogs.nytimes.com/2009/10/12/democrats-fire-back-at-insurance-industry-analysis-of-health-legislation/?hp
- The cost of the penalty is much lower than the cost of the insurance premium
- There is no pre-existing exclusion so a healthy person can wait until s/he gets sick before buying health insurance.
Here is a link to the PriceWaterhouseCoopers' report, http://graphics8.nytimes.com/packages/flash/health/pdf/pwc_report_on_Costs_final_101109.pdf
http://www.washingtonpost.com/wp-dyn/content/article/2009/10/12/AR2009101203108.html
Industry Group, White House Spar Over Premiums
By Ceci Connolly
Washington Post Staff Writer
Tuesday, October 13, 2009
Tensions between the White House and insurers exploded into open warfare Monday, with the two sides arguing over what the financial impact of comprehensive health-care legislation moving through Congress would be for average Americans.
As the Senate Finance Committee prepared to vote Tuesday on a 10-year, $829 billion bill, the insurance lobby warned that under the legislation insurance premiums could rise faster and higher than projected.
The Obama administration said the industry analysis was deeply flawed, and its allies lambasted the industry for hypocrisy and an "11th-hour attack" intended to rob President Obama of a victory on his top domestic priority.
"Health insurance companies have been laughing all the way to the bank for generations while people suffer," said Sen. John D. Rockefeller IV (D-W.Va.) "The industry stands today as the greatest impediment to real health-care reform."
The back-and-forth was reminiscent of the health-care debate of 1994, when insurers and other industry leaders helped defeat a similar effort by President Bill Clinton. On Monday, Obama advisers resurrected a report projecting similar premium increases that the industry lobby issued at the height of the Clinton-era debate to argue that the latest analysis is more of the "same old, same old" attacks.
Until now, Obama had succeeded in keeping most of the major interest groups at the bargaining table with the lure of up to 50 million new customers. But insurers have grown increasingly critical of the Finance bill, saying it does not do enough to bring healthy young people into insurance risk pools.
Although the bill would require every American to carry insurance, the committee approved changes that would postpone and reduce penalties on people who do not meet the requirement. The insurance lobby, armed with an analysis by PricewaterhouseCoopers, said that as a result, older, less-healthy patients would be more likely to buy insurance and drive up total costs.
White House budget chief Peter Orszag, citing estimates by the Congressional Budget Office, said that a new insurance marketplace, dubbed an exchange, could attract 22 million customers by 2015.
"It's hard to see how that doesn't provide adequate risk pooling and scaling," he said in an interview Monday.
Nancy-Ann DeParle, director of the White House Office of Health Reform, said the industry study overlooked other provisions of the bill that should ease premium increases. She said tax credits for small businesses and working-class families would help make insurance affordable.
Provisions that allow people to keep the insurance they have and a lower-priced plan for "young invincibles" should also hold down costs, she said.
Karen Ignagni, head of America's Health Insurance Plans, the trade group that released the report, stood by its findings. The CBO estimated that the Finance bill would cover 94 percent of legal residents by 2019, but Ignagni said insurers prefer coverage levels in the "high 90s."
PricewaterhouseCoopers predicted that new industry fees, reductions in Medicare growth and taxes on high-priced "Cadillac" policies would be costs passed on to consumers.
Orszag disputed that notion, arguing that the market will respond to those pressures by developing more affordable products.
"Almost every economist believes the effect of the Cadillac provision would be to reduce premiums over time by leading to more efficient insurance plans," he said.
Over time, a reduction in health-care spending should lead to higher wages, Orszag added.
As analysts debated the long-term effects of legislation that would restructure one-sixth of the economy, Obama's political supporters moved quickly to discredit the insurers.
Ron Pollack, executive director of the pro-reform group Families USA, said the industry report "gives hypocrisy a bad name. . . . They are like a poker player who complains about his hand when, in fact, he is the dealer."
__________
More on the dispute at:
http://www.politico.com/news/stories/1009/28213.html#
http://prescriptions.blogs.nytimes.com/2009/10/12/democrats-fire-back-at-insurance-industry-analysis-of-health-legislation/?hp
Labels:
health plan
Monday, October 12, 2009
Paying the Health Tax in Massachusetts
http://online.wsj.com/article/SB10001424052748703298004574459101022338232.html
Be warned: Even people with good insurance will risk fines if mandatory insurance becomes the national law.
By Wendy Williams, Cape Cod, Mass.
My husband retired from IBM about a decade ago, and as we aren't old enough for Medicare we still buy our health insurance through the company. But IBM, with its typical courtesy, informed us recently that we will be fined by the state.
Why? Because Massachusetts requires every resident to have health insurance, and this year, without informing us directly, the state had changed the rules in a way that made our bare-bones policy no longer acceptable. Unless we ponied up for a pricier policy we neither need nor want—or enrolled in a government-sponsored insurance plan—we would have to pay $1,000 each year to the state.
My husband's response was muted; I was shaking mad. We hadn't imposed our health-care costs on anyone else, yet we were being fined ("taxed" was the word the letter used).
We've spent much of our lives putting away what money we could for retirement. We always intended to be self-sufficient. We've paid off the mortgage on our home, don't carry credit-card debt, and have savings in case of an emergency. We also have a regular monthly income of about $3,000, which includes an IBM pension. My husband, 61, earns a little money on the side, sometimes working as an electronics consultant on renewable energy projects. I'm 58 and make some money writing science books. We are not wealthy, but we aren't a risk of becoming a burden on society either. How did we become outlaws?
The turning point was three years ago, when then-Republican Gov. Mitt Romney pushed through the state legislature a health-care plan that he promised would provide universal coverage while lifting from the middle-class the burden of having to pay for those who do not have insurance. His argument was that the uninsured drove up the cost of health care for everyone by seeking care at emergency rooms and then skipping out on their medical bills. Hospitals make up for those unpaid bills by charging everyone else more than they otherwise would.
The central plank of the Romney plan was a mandate that required everyone to buy health insurance or pay a fine for posing a risk to society by walking around without coverage. There would be subsidies for those who couldn't afford insurance, and residents would be required to buy a minimum amount of health insurance, on the grounds that they might buy a policy that doesn't cover the cost of their care and end up skipping out on their medical bills. "We insist that everybody who drives a car has insurance, and cars are a lot less expensive than people," Mr. Romney told the Boston Globe in 2006.
Mr. Romney and Sen. Ted Kennedy publicly promised that the middle class—that is, people like us—would not be taxed and that our health-care costs would actually decrease if the plan became law.
My husband and I weren't convinced. It all seemed inane, but we are neither politically or socially conservative and figured the plan wouldn't affect us much. Besides, who could be against a plan that covers more people for less money?
For the first two years of the mandate, our IBM health insurance was seen as acceptable in the eyes of the state. This year the rules changed. The state requires that health plans cap out-of-pocket expenses for individuals (not including monthly premiums) at $2,000 a year. Our plan's cap is $2,500.
Ten years ago, we had excellent coverage through a more gold-plated plan. But we found that it was no longer worth paying the premiums and scaled back to a more modest policy. Today, we pay about $300 a month for catastrophic care. If we went with the next step up in plans offered to us by IBM, our monthly premium would increase to $800. We simply don't need to pay that kind of money for the amount of health care we actually consume.
Nonetheless, we now owe the state an extra $1,000. Ironically, that's about the extra amount we would pay out-of-pocket under our current plan if both of us actually fell ill in the same year.
We could choose a state-sponsored plan. It would mean paying more than what we pay now, but less than what IBM's next step up would cost. But we don't want to.
IBM seems like a rock of stability compared to the state of Massachusetts. It's apparent that state health-care policies can change at the whim of politicians in Boston, and we might not be able to adjust to the new rules. The way we figure it, if we sign up for a state-subsidized plan we will be at the mercy of the state.
So we are sticking with our plan and paying the tax. But what bothers me most is that a similar health-care mandate is being proposed in Washington, and some of the same promises that were made here are being made again—such as that the mandate will never hit middle-class folks with a new tax. When asked about the mandate, Maine Republican Sen. Olympia Snowe said recently, according to the New York Times, "It surprises me that we would have these high-level penalties on average Americans."
Well, I don't find it surprising. The mandate in Massachusetts was sold as something that wouldn't penalize people like my husband and me. But those political promises were only good for as long as it took to get the mandate enacted into law.
Mrs. Williams is co-author of "Cape Wind: Money, Celebrity, Class, Politics and the Battle for Our Energy Future" (PublicAffairs, 2007).
Be warned: Even people with good insurance will risk fines if mandatory insurance becomes the national law.
By Wendy Williams, Cape Cod, Mass.
My husband retired from IBM about a decade ago, and as we aren't old enough for Medicare we still buy our health insurance through the company. But IBM, with its typical courtesy, informed us recently that we will be fined by the state.
Why? Because Massachusetts requires every resident to have health insurance, and this year, without informing us directly, the state had changed the rules in a way that made our bare-bones policy no longer acceptable. Unless we ponied up for a pricier policy we neither need nor want—or enrolled in a government-sponsored insurance plan—we would have to pay $1,000 each year to the state.
My husband's response was muted; I was shaking mad. We hadn't imposed our health-care costs on anyone else, yet we were being fined ("taxed" was the word the letter used).
We've spent much of our lives putting away what money we could for retirement. We always intended to be self-sufficient. We've paid off the mortgage on our home, don't carry credit-card debt, and have savings in case of an emergency. We also have a regular monthly income of about $3,000, which includes an IBM pension. My husband, 61, earns a little money on the side, sometimes working as an electronics consultant on renewable energy projects. I'm 58 and make some money writing science books. We are not wealthy, but we aren't a risk of becoming a burden on society either. How did we become outlaws?
The turning point was three years ago, when then-Republican Gov. Mitt Romney pushed through the state legislature a health-care plan that he promised would provide universal coverage while lifting from the middle-class the burden of having to pay for those who do not have insurance. His argument was that the uninsured drove up the cost of health care for everyone by seeking care at emergency rooms and then skipping out on their medical bills. Hospitals make up for those unpaid bills by charging everyone else more than they otherwise would.
The central plank of the Romney plan was a mandate that required everyone to buy health insurance or pay a fine for posing a risk to society by walking around without coverage. There would be subsidies for those who couldn't afford insurance, and residents would be required to buy a minimum amount of health insurance, on the grounds that they might buy a policy that doesn't cover the cost of their care and end up skipping out on their medical bills. "We insist that everybody who drives a car has insurance, and cars are a lot less expensive than people," Mr. Romney told the Boston Globe in 2006.
Mr. Romney and Sen. Ted Kennedy publicly promised that the middle class—that is, people like us—would not be taxed and that our health-care costs would actually decrease if the plan became law.
My husband and I weren't convinced. It all seemed inane, but we are neither politically or socially conservative and figured the plan wouldn't affect us much. Besides, who could be against a plan that covers more people for less money?
For the first two years of the mandate, our IBM health insurance was seen as acceptable in the eyes of the state. This year the rules changed. The state requires that health plans cap out-of-pocket expenses for individuals (not including monthly premiums) at $2,000 a year. Our plan's cap is $2,500.
Ten years ago, we had excellent coverage through a more gold-plated plan. But we found that it was no longer worth paying the premiums and scaled back to a more modest policy. Today, we pay about $300 a month for catastrophic care. If we went with the next step up in plans offered to us by IBM, our monthly premium would increase to $800. We simply don't need to pay that kind of money for the amount of health care we actually consume.
Nonetheless, we now owe the state an extra $1,000. Ironically, that's about the extra amount we would pay out-of-pocket under our current plan if both of us actually fell ill in the same year.
We could choose a state-sponsored plan. It would mean paying more than what we pay now, but less than what IBM's next step up would cost. But we don't want to.
IBM seems like a rock of stability compared to the state of Massachusetts. It's apparent that state health-care policies can change at the whim of politicians in Boston, and we might not be able to adjust to the new rules. The way we figure it, if we sign up for a state-subsidized plan we will be at the mercy of the state.
So we are sticking with our plan and paying the tax. But what bothers me most is that a similar health-care mandate is being proposed in Washington, and some of the same promises that were made here are being made again—such as that the mandate will never hit middle-class folks with a new tax. When asked about the mandate, Maine Republican Sen. Olympia Snowe said recently, according to the New York Times, "It surprises me that we would have these high-level penalties on average Americans."
Well, I don't find it surprising. The mandate in Massachusetts was sold as something that wouldn't penalize people like my husband and me. But those political promises were only good for as long as it took to get the mandate enacted into law.
Mrs. Williams is co-author of "Cape Wind: Money, Celebrity, Class, Politics and the Battle for Our Energy Future" (PublicAffairs, 2007).
Labels:
health plan
Subscribe to:
Posts (Atom)